Permanent Choices: A 2026 Update
Deciding on permanent birth control is a deeply personal choice. You deserve all the information to make the right decision for you and your future.
This guide covers sterilization procedures as we head into 2026. We'll discuss common methods like tubal ligation and vasectomy, along with less frequent options. You'll learn what each procedure involves, recovery expectations, and potential risks and benefits.
We'll also cover insurance coverage, costs, and legal requirements. Sterilization laws evolve, so staying informed is important. Access to reproductive healthcare is complex, and we'll discuss finding a supportive provider.
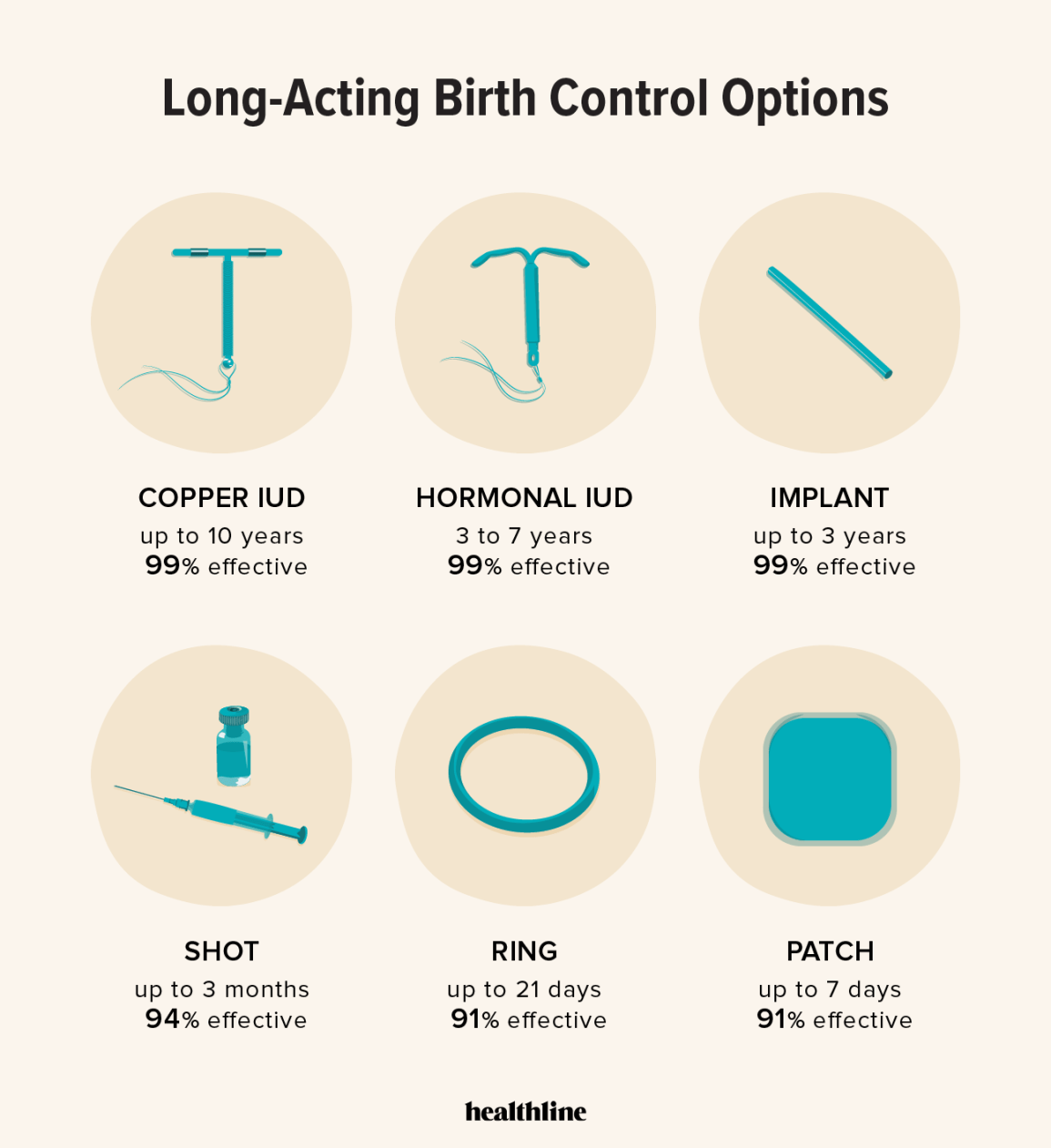
Tubal Ligation: The Traditional Route
Tubal ligation, or "getting your tubes tied," is a surgery that prevents pregnancy by blocking or removing the fallopian tubes. It's a common and effective permanent birth control method. Surgeons use several techniques for this procedure.
The methods include burning (cauterization), banding (using clips to close the tubes), clipping (applying titanium clips), and resection (removing a section of the tubes). The choice of method often depends on your individual anatomy and your surgeon’s preference. Resection is becoming more common due to its slightly higher effectiveness and potential to reduce the risk of ectopic pregnancy.
Recovery time is typically fairly quick. Most people can return to normal activities within a week, although some mild pain and discomfort are to be expected. According to the CDC, the success rate of tubal ligation is over 99% – meaning fewer than 1 in 100 women will become pregnant within 10 years. However, it’s important to be aware of the small risk of ectopic pregnancy if the procedure fails.
Rare complications can include infection, bleeding, and damage to other organs. Discuss these risks with your doctor. Tubal ligation doesn't protect against sexually transmitted infections, so safe sex practices remain important.
- Burning (Cauterization): Uses heat to seal the tubes.
- Banding: Applies small clips to close off the tubes.
- Clipping: Uses titanium clips to block the tubes.
- Resection: Removes a section of the fallopian tubes.
UK woman wins right to receive permanent birth control after exposing double standards in health service - CNN https://t.co/Ol9cSjOy6G
— News Hub (@NewsHubGlobe) May 3, 2026
Follow @NewsHubGlobe for 24/7 breaking news from around the world. pic.twitter.com/aAsQoFNZzh
Vasectomy: For Partners & Individuals
Vasectomy is a surgery for males that prevents pregnancy by cutting or blocking the vas deferens, the tubes carrying sperm. It's simpler and less invasive than tubal ligation, with a quicker recovery. It's a valid choice for anyone who knows they don't want biological children, regardless of relationship status.
There are two main techniques: the no-scalpel vasectomy and the conventional incision method. The no-scalpel technique uses a small clamp to access the vas deferens through a tiny puncture in the scrotum, minimizing bleeding and discomfort. The conventional method involves a small incision. Both are typically performed under local anesthesia.
Recovery usually involves a few days of rest and ice packs to reduce swelling. Most men can return to work and normal activities within a week. Potential complications are relatively rare but can include pain, swelling, infection, and a small chance of sperm granuloma (a small lump that forms near the vasectomy site).
The success rate of vasectomy is over 99%. It takes several months and ejaculations to clear remaining sperm, so contraception is still needed for a time after the procedure. A common misconception is that vasectomy affects masculinity or libido, which is false. It only affects sperm count, not hormone levels or sexual function.
- No-Scalpel Vasectomy: Minimally invasive, using a small clamp.
- Conventional Incision Method: Involves a small surgical cut.
Emerging Options: Hysterectomy & Salpingectomy
Hysterectomy, the surgical removal of the uterus, can result in sterilization but is usually reserved for treating conditions like fibroids, endometriosis, or uterine cancer. It's not typically performed solely for sterilization due to significant recovery and potential complications. Types include total (removing the uterus and cervix) and partial (removing only the uterus).
Salpingectomy, the removal of the fallopian tubes, is gaining traction as a sterilization option. It eliminates the risk of ectopic pregnancy. Studies suggest salpingectomy can reduce ovarian cancer risk, as many ovarian cancers start in the fallopian tubes. It can be performed laparoscopically, minimizing recovery time.
Salpingectomy prevents pregnancy and reduces cancer risk, even with a uterus. Hysterectomy is a more extensive surgery with broader health implications. Discuss these procedures with a healthcare provider to determine the best option for your circumstances.
Navigating Insurance & Cost in 2026
The cost of sterilization varies significantly by insurance plan and location. Most insurance companies cover sterilization procedures, but coverage differs by plan and state regulations. Check with your insurance provider for details on deductibles, copays, and pre-authorization requirements.
Out-of-pocket costs can range from a few hundred dollars to several thousand, depending on the procedure, location, and whether you have insurance. Tubal ligation is generally more expensive than vasectomy due to it being a more complex surgery. Costs can include the surgeon’s fee, anesthesia fees, and facility fees.
If you lack insurance or it doesn't cover the procedure, resources are available. Some clinics offer lower-cost sterilization services, and financial assistance programs may exist. Medi-Cal, California’s Medicaid program, has specific billing instructions for sterilization services on their website (mcweb.apps.prd.cammis.medi-cal.ca.gov).
Ask for a detailed cost estimate from your provider before the procedure. Understanding the financial implications upfront helps you make an informed decision.
Comparing Permanent Sterilization Options (Estimated Costs & Key Considerations - 2026)
| Procedure | Typical Recovery | Cost with Insurance | Cost without Insurance | Notes |
|---|---|---|---|---|
| Tubal Ligation (Tubes Tied) | Generally a few days to a week. | Often covered, potentially a copay or deductible. | Moderate to High | Historically common, but increasingly replaced by salpingectomy. Coverage can vary by plan. |
| Bilateral Salpingectomy (Tube Removal) | Similar to tubal ligation – a few days to a week. | Often covered, potentially a copay or deductible. | Moderate to High | Offers slight risk reduction for ovarian cancer in addition to permanent contraception. |
| Vasectomy (Male Sterilization) | Typically a few days, often back to normal activity within a week. | Often covered, potentially a copay or deductible. | Low to Moderate | Generally considered a simpler procedure with quicker recovery than female sterilization options. |
| Hysterectomy (Uterus Removal) | Several weeks to months, depending on approach (vaginal, laparoscopic, abdominal). | Coverage dependent on medical necessity; may require pre-authorization. | High | This is a major surgery and is *not* solely for contraception. Often considered for other health reasons alongside sterilization. |
| Essure (Cystourethral Device - *Discontinued*) | N/A - Procedure no longer offered. | N/A | N/A | Important note: Essure is no longer available due to complications. This is included for awareness as some individuals may still have the device. |
| Postpartum Tubal Ligation | Potentially faster recovery if done immediately after childbirth. | Often covered when performed during a C-section or immediately postpartum. | Moderate to High | Convenient timing for some, but requires careful consideration during the postpartum period. |
Qualitative comparison based on the article research brief. Confirm current product details in the official docs before making implementation choices.
Legal Considerations & Informed Consent
Informed consent is a crucial part of sterilization. Doctors must provide comprehensive information about the procedure, including risks, benefits, alternatives, and potential long-term effects. This information should be understandable, and you should have ample opportunity to ask questions.
Some states have waiting periods or require counseling before sterilization. These laws ensure the decision is made thoughtfully and voluntarily. Be aware of your state's requirements. Some states also have age restrictions or require spousal consent, though these are less common.
Historical instances of forced or coerced sterilization have targeted marginalized communities. Find a provider who respects your autonomy and doesn't pressure you. If you feel pressured or uncomfortable, seek a second opinion.
If you encounter legal challenges or restrictions to sterilization access, resources like the ACLU and Planned Parenthood can provide legal assistance and advocacy.
Finding a Supportive Provider
Find a doctor who is respectful, non-judgmental, and knowledgeable about sterilization options. You want a provider who listens to your concerns, answers questions honestly, and supports your decision. Don't settle for a doctor who dismisses your feelings or steers you toward a different choice.
undefined
Pay attention to how the doctor makes you feel. Do they listen attentively? Do they explain things clearly? Do you feel comfortable and respected? If you have any doubts, don’t hesitate to seek a second opinion. It’s your body, and you deserve to feel empowered and confident in your healthcare choices.
If a provider is dismissive, condescending, or tries to dissuade you from sterilization without a valid medical reason, that’s a red flag. Don’t be afraid to advocate for yourself and find a doctor who is truly supportive.
Common Sterilization Procedures - Overview (2026)
| Procedure | Typical Candidate | Key Considerations | Reversibility |
|---|---|---|---|
| Tubal Ligation (for people with uteruses) | Individuals who have completed childbearing and desire permanent contraception. | Generally performed laparoscopically or after childbirth. Recovery time varies. | Reversal is possible, but not always successful. Success rates depend on the type of ligation and individual factors. |
| Vasectomy (for people with testicles) | Individuals who have completed childbearing and desire permanent contraception. | A minimally invasive procedure performed in a doctor's office or clinic. Generally quick recovery. | Reversal is possible, but can be complex and is not always successful. Success rates vary. |
| Hysterectomy (removal of the uterus) | Individuals with specific medical conditions (like fibroids, endometriosis, or cancer) *or* those who definitely do not want future pregnancies. | A major surgical procedure with a longer recovery period. Can be performed in various ways (abdominal, vaginal, laparoscopic). | Permanent - eliminates the possibility of pregnancy. |
| Oophorectomy (removal of the ovaries) | Individuals with specific medical conditions or a high risk of ovarian cancer. *Not* typically performed solely for sterilization. | A surgical procedure with potential hormonal consequences. Often performed alongside hysterectomy. | Permanent - eliminates the possibility of pregnancy and natural hormone production. |
| Essure (discontinued, but relevant for those who have had the procedure) | Individuals who previously opted for this non-surgical tubal ligation method. | Essure is no longer available, but some individuals still have the implants. Potential for complications has been reported. | Not easily reversible. Removal may be required in some cases due to complications. |
| Salpingectomy (removal of fallopian tubes) | Individuals seeking permanent contraception and potentially reducing the risk of ovarian cancer. | Can be performed laparoscopically. Offers a potentially higher degree of effectiveness than tubal ligation. | Permanent - eliminates the possibility of pregnancy. |
Illustrative comparison based on the article research brief. Verify current pricing, limits, and product details in the official docs before relying on it.
Life After Sterilization: Emotional & Social Aspects
Choosing permanent birth control can bring a range of emotions. Many people experience a sense of relief and empowerment, knowing they have taken control of their reproductive future. Others may experience feelings of grief, especially if they once envisioned having children. It’s okay to feel a mix of emotions – there’s no right or wrong way to feel.
Navigating conversations with family and friends can be challenging. Some people may be supportive, while others may not understand your decision. Be prepared to explain your reasons and set boundaries. You don’t owe anyone an explanation, but having a prepared response can help you handle difficult conversations.
Remember that choosing sterilization doesn’t diminish your worth or value as a person. It’s a personal decision that should be respected. Surround yourself with supportive people who understand and accept your choice.
There are online communities and support groups where you can connect with others who have made the same decision. Sharing your experiences and connecting with like-minded individuals can be incredibly validating.
How did you feel emotionally in the months following your sterilization?
Vote below!

No comments yet. Be the first to share your thoughts!