Making the Choice: A Personal Decision
Deciding to pursue sterilization is a deeply personal one, often arrived at after considerable thought and self-reflection. It's a decision that deserves respect and understanding, free from societal expectations or judgment. For many, it represents an affirmation of their current life stage and a proactive step towards aligning their reproductive choices with their long-term goals.
There's a growing movement of individuals choosing to live childfree, and with that comes an increased openness around sterilization as a permanent form of birth control. While statistics vary, data suggests a consistent interest in these procedures; a 2023 study by the Guttmacher Institute showed that interest in sterilization increased during periods of reproductive rights uncertainty.
This isn’t a decision to be taken lightly. It’s important to acknowledge the emotional weight involved, and to fully understand the implications. The goal is informed consent – being fully aware of the procedure, its risks, benefits, and alternatives – so you can make a choice that feels right for you.
Framing this decision as empowering is essential. It’s not about regret or closing doors, but about intentionally creating the life you desire. Open communication with your partner, if applicable, is also key. A shared understanding and mutual support can strengthen your relationship as you navigate this significant life choice.
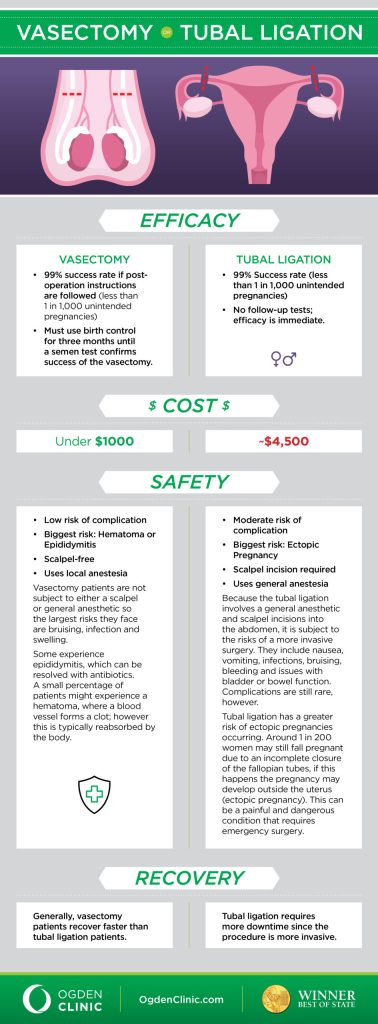
Tubal Ligation: Methods and What to Expect
Tubal ligation, often referred to as "getting your tubes tied," is a surgical procedure that prevents pregnancy by blocking or removing the fallopian tubes. There are several methods to accomplish this, each with its own nuances. Banding involves applying a clip-like band to the tubes, causing them to close off. Clipping utilizes small clamps to block the tubes.
Burning, or cauterization, uses heat to seal the tubes. Resection, a more definitive approach, involves cutting and removing a section of the fallopian tubes. The method chosen often depends on factors like the patient’s medical history, surgeon preference, and whether the procedure is performed during a Cesarean section.
Most tubal ligations are now performed laparoscopically, meaning through small incisions in the abdomen using a camera and specialized instruments. This results in less pain and a faster recovery compared to traditional open surgery. General or regional anesthesia is typically used during the procedure.
Recovery time varies, but most individuals can return to light activity within a week. Expect some pain and discomfort, which can usually be managed with over-the-counter pain medication. More strenuous activity should be avoided for several weeks. Potential complications, though rare, include infection, bleeding, and damage to other organs. The success rate of tubal ligation is over 99% but failure, though uncommon, can result in ectopic pregnancy.
It's important to discuss all available methods with your surgeon to determine which is the best fit for your individual circumstances. Don't hesitate to ask questions about the risks, benefits, and recovery process. Understanding these details will empower you to make an informed decision.
Vasectomy: A Simpler Path?
A vasectomy is a surgical procedure for men that prevents pregnancy by cutting or blocking the vas deferens, the tubes that carry sperm. It's generally considered a simpler and less invasive procedure than tubal ligation, often performed in a doctor's office or clinic setting.
The procedure typically uses local anesthesia, meaning you’ll be awake but the area will be numbed. There are two main techniques: the "no-scalpel’ vasectomy, which involves making a small puncture in the scrotum to access the vas deferens, and the traditional method, which involves a small incision. The ‘no-scalpel" approach is becoming increasingly popular due to its reduced risk of bleeding and faster recovery.
Recovery is relatively quick. Expect some pain, swelling, and bruising in the scrotum, which can be managed with ice packs and over-the-counter pain medication. Most men can return to light activity within a few days, but strenuous activity should be avoided for about a week. It's crucial to follow your doctor’s instructions regarding activity restrictions.
A key component of post-vasectomy care is semen analysis. Multiple samples are collected over several months to confirm the absence of sperm, ensuring the procedure was successful. It’s vital to continue using contraception until your doctor confirms sterility. The success rate of vasectomy is exceptionally high, exceeding 99%. Potential complications include pain, swelling, infection, hematoma, and, rarely, post-vasectomy pain syndrome.
While generally safe, it's important to be aware of potential risks and to choose a qualified and experienced surgeon. Discuss any concerns you have with your doctor before proceeding.
Cost Breakdown: 2026 Estimates
The cost of sterilization procedures can vary significantly based on location, the surgeon’s fees, anesthesia costs, and facility fees. As of late 2023/early 2024, and projecting into 2026, a tubal ligation can range from $3,000 to $8,000, while a vasectomy typically costs between $700 and $3,000.
Surgeon's fees generally make up the largest portion of the cost, ranging from $1,500 to $5,000 for tubal ligation and $500 to $2,000 for vasectomy. Anesthesia fees can add another $500 to $1,500, and facility fees (hospital or surgical center) can range from $1,000 to $3,000. Don’t forget to factor in the cost of follow-up appointments, which can add several hundred dollars.
Costs are typically higher in urban areas compared to rural areas. For example, a tubal ligation in New York City might cost $6,000-$8,000, while the same procedure in a rural area of the Midwest could cost $3,000-$5,000. Insurance coverage varies widely. Many insurance plans cover sterilization procedures as preventative care, but some may require pre-authorization or have high deductibles.
Navigating pre-authorization can be complex. It’s best to contact your insurance provider directly to understand your coverage and any requirements. Financing options and payment plans are available through some providers and healthcare financing companies. Look into options like CareCredit or other medical loan providers to help manage the costs.
Comparing Sterilization Options: Tubal Ligation vs. Vasectomy (2026)
| Feature | Tubal Ligation | Vasectomy |
|---|---|---|
| Cost | Medium to High | Low to Medium |
| Invasiveness | High | Low |
| Recovery Time | Medium (Several days to weeks) | Low (Few days) |
| Reversibility | Low (Surgical repair possible, but not always successful) | Medium (Surgical repair often successful, but not guaranteed) |
| Procedure Location | Hospital or Surgical Center | Doctor's Office or Clinic |
| Anesthesia | Typically General or Regional | Typically Local |
| Long-Term Health Risks | Low (Potential for post-operative infection, ectopic pregnancy if failure occurs) | Low (Potential for post-operative pain, infection, or hematoma) |
| Effectiveness | High (Over 99%) | High (Over 99%) |
Illustrative comparison based on the article research brief. Verify current pricing, limits, and product details in the official docs before relying on it.
Reversibility: Options and Realities
While sterilization is generally considered a permanent form of birth control, reversal procedures are available. However, it’s crucial to understand that reversal is not guaranteed and should not be the primary reason for choosing sterilization. Success rates vary depending on several factors.
For tubal ligation reversal, success rates range from 40% to 80%, depending on factors like the length of the blocked tubes, the patient’s age, and the surgeon’s experience. A shorter segment of blocked tube generally leads to a higher success rate. For vasectomy reversal, success rates are generally higher, ranging from 75% to 95%, again depending on factors like the time since vasectomy and the surgeon’s skill.
The cost of reversal procedures is significant. Tubal ligation reversal can cost between $8,000 and $20,000, while vasectomy reversal typically ranges from $5,000 to $15,000. These costs can vary based on location, surgeon’s fees, and the complexity of the procedure.
It’s vital to have realistic expectations about reversal. Even with a successful reversal, there’s no guarantee of pregnancy. The procedure should be viewed as an option, not a certainty. Thoroughly discuss the risks, benefits, and costs with a qualified surgeon before making a decision.
When considering sterilization, how important was the possibility of reversal to your decision?
As childfree individuals, we know this decision carries weight. Whether you have already been sterilized or are currently researching your options, we want to hear from you. Your response helps our community understand the real priorities behind this deeply personal choice. Vote below!
Potential Risks and Complications
As with any surgical procedure, both tubal ligation and vasectomy carry potential risks and complications. For tubal ligation, these include ectopic pregnancy (if the procedure fails), infection, bleeding, and damage to other organs during surgery. While rare, these complications can be serious and may require additional medical intervention.
Vasectomy also carries risks, including pain, swelling, infection, hematoma (blood collection in the scrotum), and post-vasectomy pain syndrome (chronic testicular pain). Post-vasectomy pain syndrome is a relatively uncommon complication, but it can be debilitating for those affected.
The CDC provides guidelines for sterilization safety to minimize the risk of infection and other complications. These guidelines emphasize the importance of proper surgical technique, sterile equipment, and appropriate post-operative care. Choosing a surgeon who adheres to these guidelines is crucial.
It’s essential to discuss these risks with your surgeon and to understand what to look for in terms of potential complications. Knowing the signs of infection or other problems can help you seek prompt medical attention if needed. Open communication with your healthcare provider is key to managing any potential complications.
Finding the Right Provider
Choosing a qualified and experienced surgeon is paramount. Look for a board-certified gynecologist for tubal ligation and a board-certified urologist for vasectomy. Check their credentials and ensure they have extensive experience performing the procedure you’re considering.
During a consultation, ask questions about their experience, success rates, complication rates, and preferred surgical techniques. It’s also important to find a provider who is supportive and non-judgmental, and who respects your decision. Don't hesitate to seek a second opinion if you feel uncomfortable or unsure.
Resources for finding providers include the American College of Obstetricians and Gynecologists (ACOG) and urology associations. Online reviews and patient testimonials can also provide valuable insights. Trust your instincts and choose a provider you feel confident in.
Essential Post-Sterilization Recovery Kit

Seamless wireless design for ultimate comfort · Full coverage support for nursing mothers · Soft, breathable fabric for all-day wear
This nursing bra offers exceptional comfort and support, crucial for a smooth recovery period.

Instant cold therapy for effective pain relief · Disposable and convenient for immediate use · Ideal for reducing swelling and inflammation
These instant ice packs provide rapid relief from pain and swelling, aiding in a comfortable recovery.

Topical gel for fast-acting pain relief · Reduces swelling and bruising from injuries · Non-greasy and fragrance-free formula
Arnicare Gel effectively soothes muscle soreness and swelling, promoting a quicker return to daily activities.

Soft cotton construction for breathability · Low-impact support for everyday comfort · OEKO-TEX STANDARD 100 certified for safety
These cotton bralettes provide gentle, comfortable support, ideal for relaxed recovery at home.

Lightweight knit jersey for superior comfort · Jogger style for relaxed fit · Breathable fabric for all-night wear
These pajama pants ensure maximum comfort and ease of movement during your recovery downtime.
As an Amazon Associate I earn from qualifying purchases. Prices may vary.
Beyond the Procedure: Emotional Wellbeing
Sterilization can have a significant emotional impact. Some individuals experience relief and a sense of empowerment, while others may grapple with feelings of grief, uncertainty, or even regret. It's important to acknowledge these emotions and to allow yourself time to process them.
If you’re struggling with the emotional aftermath of sterilization, consider seeking support from a therapist, joining a support group, or connecting with online communities. Open communication with your partner is also crucial. Remember, your feelings are valid, and it’s okay to ask for help.


No comments yet. Be the first to share your thoughts!