Your Childfree Birth Control Toolkit
Choosing not to have children is a deeply personal decision, and with that decision comes the responsibility – and the right – to proactively manage your reproductive health. This isn't about restriction; it's about empowerment. It’s about taking control of your body and your future, and living the life you want, free from unintended pregnancy. For many childfree individuals, that means selecting a highly effective contraception method.
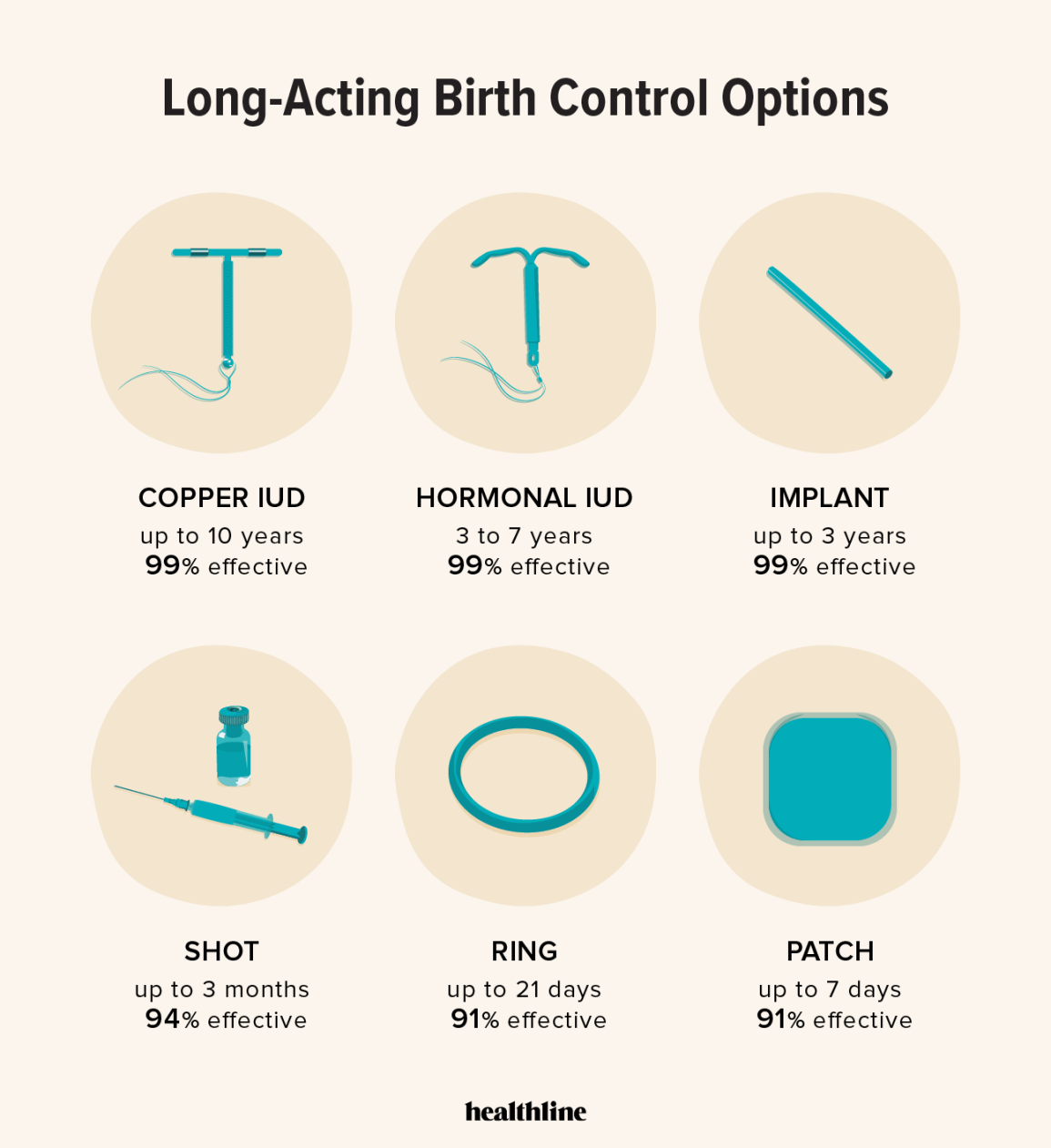
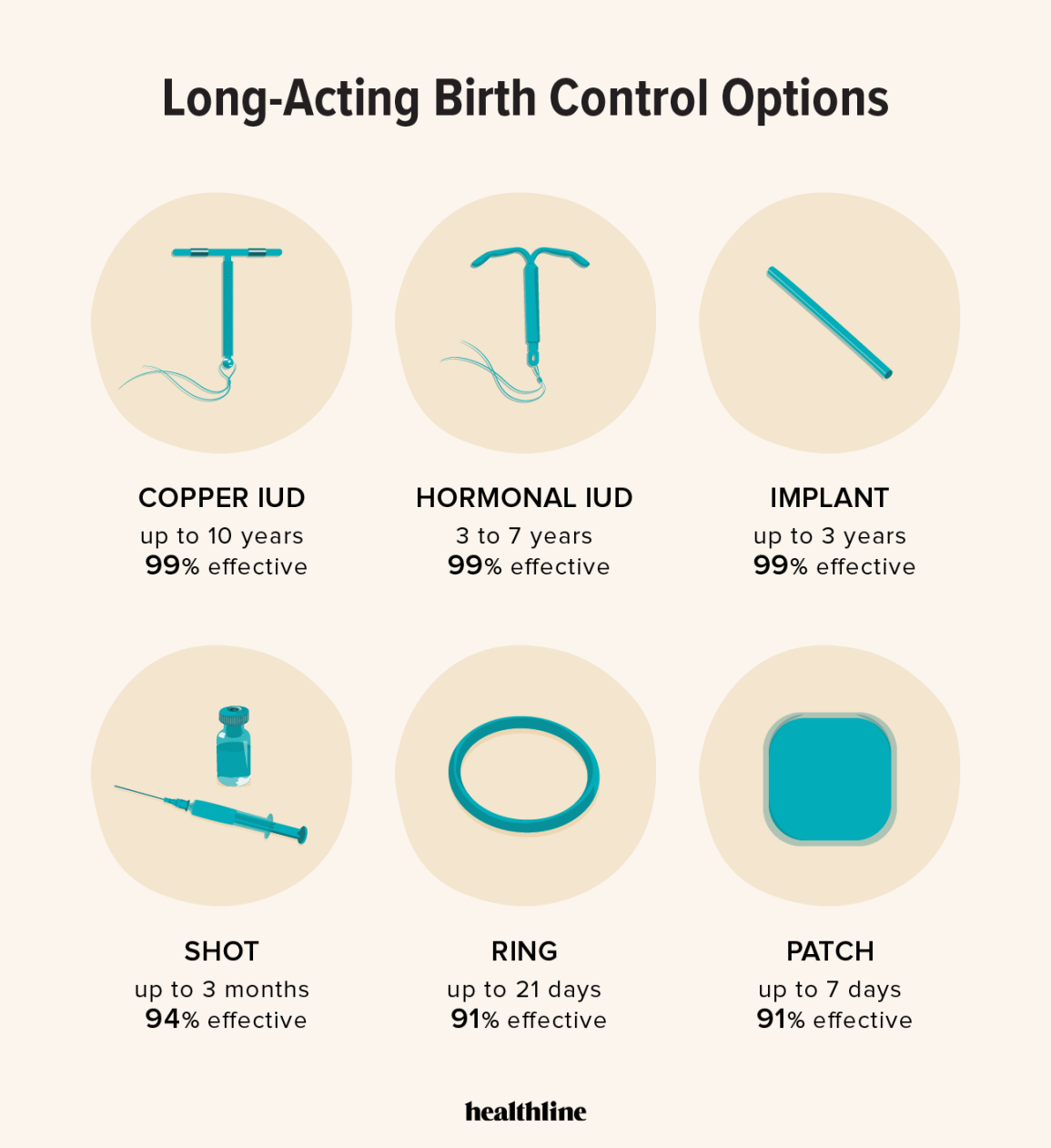
Long-term reversible contraception (LARC) methods are particularly popular among those who are certain about not wanting children. This isn't surprising. Options like IUDs and implants offer convenience, with set-it-and-forget-it reliability for years at a time. This reduces the mental load of daily or monthly contraception management, allowing you to focus on the things that matter most to you.
The sheer variety of options can feel overwhelming, but understanding the nuances of each method is essential. We’ll move beyond the basic descriptions often provided and address the realities – the benefits, the potential side effects, and the practical considerations – so you can make an informed decision that aligns with your lifestyle and priorities. This guide is designed to give you the information you need to confidently discuss your options with your healthcare provider.
IUDs: The Copper and Hormonal Options
Intrauterine Devices, or IUDs, are one of the most effective forms of reversible birth control available. They are small, T-shaped devices inserted into the uterus by a healthcare professional. There are two main types: copper IUDs and hormonal IUDs. The copper IUD, Paragard, is hormone-free and works by creating an inflammatory response that is toxic to sperm, preventing fertilization.
Hormonal IUDs – Mirena, Kyleena, Liletta, and Skyla – release progestin, a synthetic form of progesterone. This thickens cervical mucus, making it difficult for sperm to reach the egg, and can also thin the uterine lining. According to the CDC, IUDs are over 99% effective at preventing pregnancy. However, effectiveness can drop slightly with typical use, accounting for user error (though with IUDs, there is very little user error!).
Insertion can be uncomfortable, and many providers recommend taking an over-the-counter pain reliever beforehand. Some people experience cramping or spotting after insertion, which usually subsides within a few days. More serious, though rare, complications include expulsion (the IUD coming out of place) and uterine perforation. Expulsion rates vary, but are generally low – around 2-5% within the first year. If expulsion occurs, you should contact your healthcare provider immediately.
Side effects differ between the types. Copper IUDs can sometimes lead to heavier, longer periods and increased cramping. Hormonal IUDs often lighten periods, and some users experience amenorrhea (no periods at all). It’s important to note that hormonal IUDs still contain hormones, and some individuals may experience hormone-related side effects like mood changes or acne. All IUDs offer 5-10 years of contraception, depending on the brand, and can be removed at any time.
- Paragard (Copper IUD): Hormone-free, effective for up to 10 years.
- Mirena: Releases a higher dose of progestin, effective for up to 8 years; often used to treat heavy bleeding.
- Kyleena: Releases a lower dose of progestin than Mirena, effective for up to 5 years.
- Liletta: Similar to Kyleena, effective for up to 8 years.
- Skyla: Releases the lowest dose of progestin, effective for up to 3 years.
Intrauterine Device (IUD) Comparison for Childfree Women - 2026
| Hormone Type | Hormone Dosage | Lifespan | Typical Failure Rate (over 5 years) | Common Side Effects | Approximate Cost (USD, as of 2026) |
|---|---|---|---|---|---|
| Levonorgestrel | 52 mg | Up to 8 years | 0.2% | Irregular bleeding or spotting (especially in the first 3-6 months), lighter periods over time, possible mood changes, acne. | $800 - $1300 (including insertion) |
| Levonorgestrel | 19.5 mg | Up to 5 years | 0.2% | Lighter periods, potentially reduced menstrual cramping, irregular bleeding or spotting (especially in the first 3-6 months), possible mood changes. | $700 - $1100 (including insertion) |
| Levonorgestrel | 38 mg | Up to 8 years | 0.2% | Lighter or absent periods, irregular bleeding or spotting (especially in the first 3-6 months), possible mood changes. | $800 - $1200 (including insertion) |
| Levonorgestrel | 14 mg | Up to 3 years | 0.2% | Irregular bleeding or spotting (especially in the first 3-6 months), lighter periods, possible mood changes. | $700 - $1000 (including insertion) |
| Copper | None (hormone-free) | Up to 10 years | 0.2% | Heavier, longer, and potentially more painful periods, possible increased cramping, spotting between periods. | $900 - $1400 (including insertion) |
Illustrative comparison based on the article research brief. Verify current pricing, limits, and product details in the official docs before relying on it.
The Implant: Nexplanon Reviewed
Nexplanon is a small, flexible rod inserted under the skin of your upper arm by a healthcare provider. It releases progestin, similar to hormonal IUDs, preventing pregnancy by thickening cervical mucus and suppressing ovulation. The CDC reports Nexplanon is over 99% effective, making it one of the most reliable contraceptive options available.
Insertion and removal are relatively quick procedures, typically taking only a few minutes. You’ll receive local anesthesia to numb the area, but some discomfort is common. A common side effect is irregular bleeding, which can be unpredictable for the first few months. Other potential side effects include mood changes, weight gain, and headaches, though these vary greatly from person to person.
One of the biggest advantages of Nexplanon is its reversibility. Once the implant is removed after three years, your fertility returns relatively quickly. It's a good choice for those who want highly effective contraception without a long-term commitment. However, if you have a history of depression or significant mood disorders, you should discuss the potential risks with your doctor.
- Effectiveness: Over 99%
- Lifespan: 3 years
- Reversibility: Fertility returns quickly after removal
- Common Side Effects: Irregular bleeding, mood changes, weight gain
Hormonal Injections: Depo-Provera
Depo-Provera is a hormonal injection administered every three months by a healthcare provider. It contains progestin and prevents pregnancy by suppressing ovulation and thickening cervical mucus. It’s highly effective, with a failure rate of around 4% with typical use, but requires consistent adherence to the injection schedule.
The most significant drawback of Depo-Provera is its potential side effects. While some users experience no issues, others report irregular bleeding, weight gain, mood changes, and, most concerningly, potential bone density loss. The FDA has issued a black box warning regarding the long-term use of Depo-Provera and its impact on bone mineral density. This bone density loss may not be fully reversible after stopping the injections.
Depo-Provera can also delay the return of fertility, sometimes taking up to a year or more after stopping the injections to conceive. Because of these concerns, Depo-Provera is falling out of favor with many healthcare providers and is often not recommended for long-term use. It might be considered for individuals who cannot reliably use other methods, but a thorough discussion of the risks and benefits is essential.
Sterilization: Permanent Options
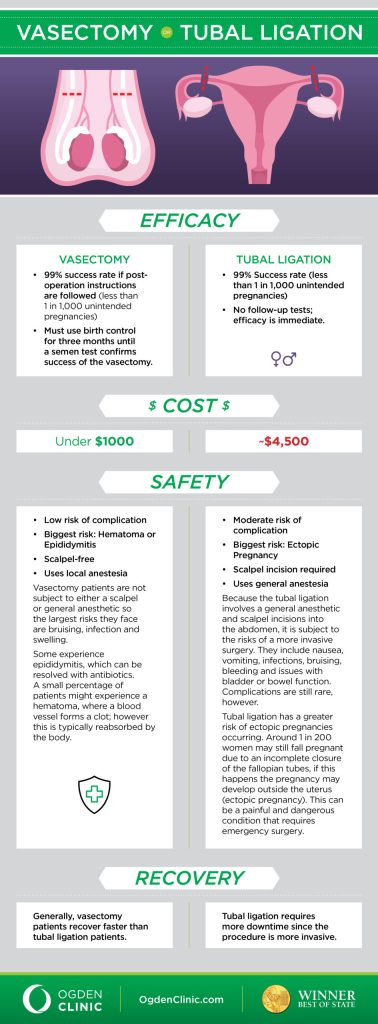
Sterilization is a permanent form of birth control and should be considered only if you are absolutely certain you do not want to have children in the future. For those with a uterus, tubal ligation involves blocking or removing the fallopian tubes, preventing the egg from reaching the uterus. For partners with sperm, vasectomy involves blocking or cutting the vas deferens, preventing sperm from being released in semen.
Tubal ligation is typically performed laparoscopically, requiring a short recovery period. Vasectomy is a simpler procedure performed in a doctor's office with local anesthesia, and recovery is usually quick. Both procedures are highly effective, with failure rates of less than 1%. However, it’s crucial to understand that sterilization is not always reversible.
Tubal reversal surgery is available, but it’s not always successful, and success rates depend on factors like the extent of the initial ligation and the individual's anatomy. Vasectomy reversal is generally more successful, but still doesn’t guarantee fertility. It's essential to discuss the potential for regret with your healthcare provider before undergoing sterilization. Consider the emotional and psychological implications of a permanent decision.
- Tubal Ligation: Permanent blocking or removal of fallopian tubes.
- Vasectomy: Permanent blocking or cutting of the vas deferens.
- Effectiveness: Over 99%
- Reversibility: Not always successful; consider carefully.
New & Emerging Long-Acting Contraception
Research into new contraceptive technologies is ongoing, with several promising options in development. One area of focus is the development of new vaginal rings that release hormones over longer periods, potentially lasting for a year or more. Researchers are also exploring new types of IUDs with improved delivery systems and reduced side effects.
Another area of interest is the development of male hormonal contraception. While a vasectomy is highly effective, many men are hesitant to undergo a permanent procedure. Researchers are working on hormonal injections and gels that could temporarily suppress sperm production. These options are still in clinical trials, but they represent a potential breakthrough in male contraception. It’s important to manage expectations; these technologies are not yet widely available.
Navigating Cost and Access
The cost of long-term contraception can vary significantly depending on your insurance coverage and the method you choose. IUDs and implants typically have higher upfront costs, but they are often covered by insurance. Depo-Provera injections are generally more affordable per dose, but the ongoing cost can add up over time. Sterilization procedures may also be covered by insurance, but this varies.
For individuals without insurance or with limited coverage, resources like Title X-funded clinics and Planned Parenthood can provide affordable contraception options. These clinics offer a sliding fee scale based on income. You can find a local clinic by visiting the Planned Parenthood website or the Office of Population Affairs website. It's important to advocate for your reproductive health and seek out resources to ensure you have access to the contraception you need.
Comfort Essentials for IUD Insertion and Removal

Provides cold therapy for swelling and pain relief · Designed for ankle, foot, heel, and arch support · Offers compression for sprains and tendonitis
This ankle ice pack wrap offers targeted cold therapy and compression to alleviate discomfort and swelling that may occur post-IUD insertion.

Formulated for women's skin · Dermatologist-tested and hypoallergenic · Designed for balancing skin
This skin cream is recommended for its potential to support skin health and comfort, which can be beneficial during hormonal changes or recovery periods.

Seamless wireless design for comfort · Provides full coverage · Suitable for nursing and maternity
While designed for nursing, the seamless and supportive nature of this bra can offer comfort and gentle support during recovery periods.

Absorbent period underwear · Comfort-stretch design · Holds up to 12 regular tampons' worth of flow
These period underwear offer a comfortable and reliable alternative for managing menstrual flow, providing discretion and ease of use.
As an Amazon Associate I earn from qualifying purchases. Prices may vary.
Talking to Your Doctor
Having an open and honest conversation with your healthcare provider is crucial when choosing a contraception method. Don't be afraid to ask questions and express your concerns. Prepare a list of questions beforehand, including questions about effectiveness, side effects, and cost. Be clear about your desire to avoid pregnancy and your preferences for a long-term, reliable method.
If you encounter a provider who is dismissive of your choices or doesn't provide you with adequate information, don't hesitate to seek a second opinion. You deserve to have a healthcare provider who respects your autonomy and supports your reproductive health decisions. Remember, you are the expert on your own body and your own life.


No comments yet. Be the first to share your thoughts!