Beyond the Basics: Why Long-Term Matters
Let’s be real: remembering to take a pill every single day is a drag. And for those of us intentionally building a childfree life, that daily reminder can feel…a little stressful. It's about wanting to feel secure in your choices, and not constantly worrying about potential slip-ups. Most of us chose this path with intention, and that deserves a birth control method that respects that intention.
Many women find themselves moving beyond the pill, not because it's ineffective, but because of the convenience factor. It's the freedom of 'set it and forget it,' knowing you're covered for years at a time. This can be a huge emotional weight off your shoulders, allowing you to focus on other things – your career, your relationships, your travels, your passions – without that constant background anxiety.
Choosing a long-term method isn’t just about preventing pregnancy; it’s about taking control of your reproductive health and aligning your birth control with your lifestyle. It’s about peace of mind and the ability to live fully, knowing you’re prepared. For many in the childfree community, that feeling of control is incredibly empowering.
The IUD Landscape: Hormonal vs. Copper
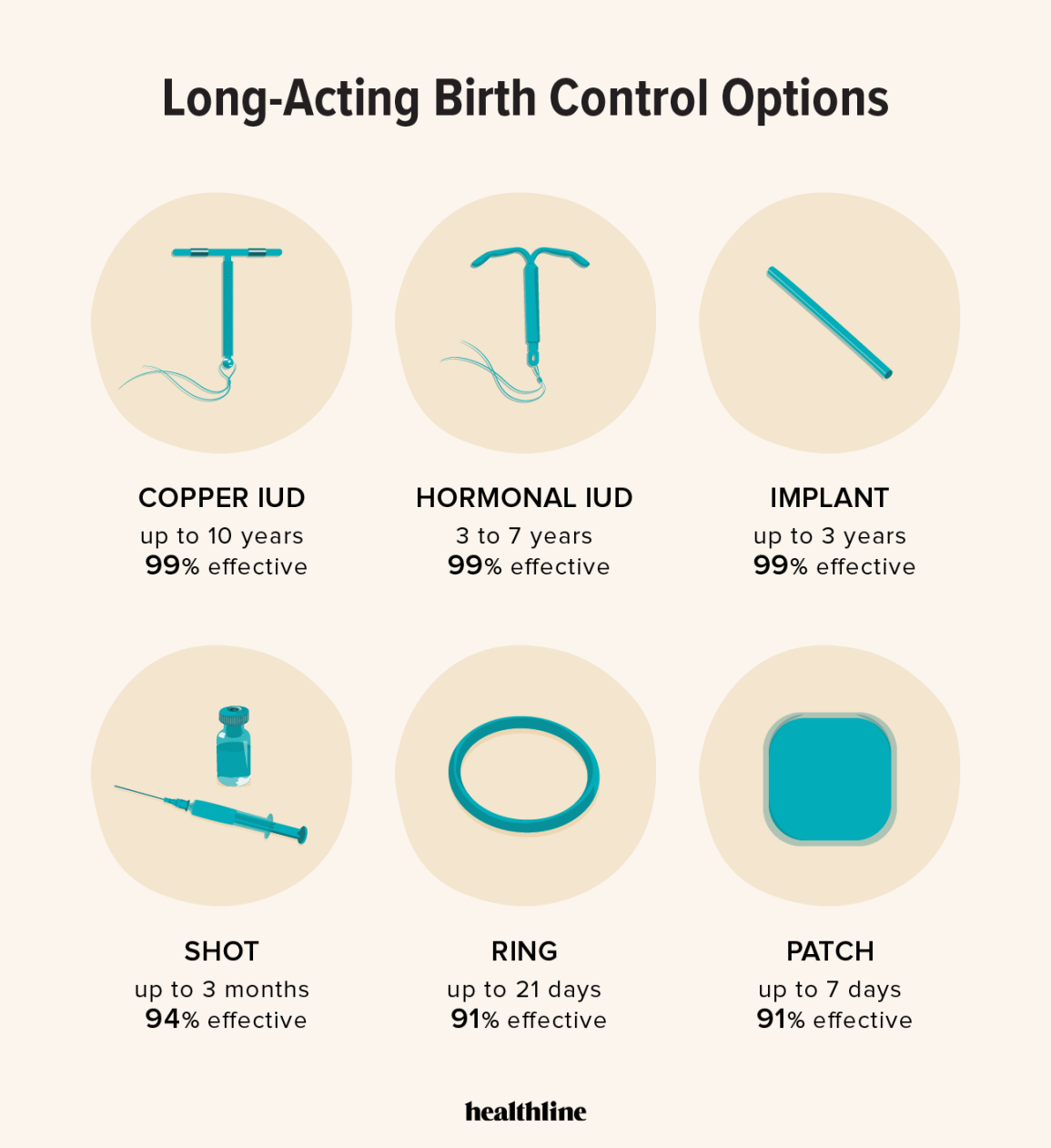
Intrauterine devices, or IUDs, are one of the most effective forms of reversible birth control available. They’re small, T-shaped devices inserted into the uterus by a healthcare provider. They work by preventing fertilization, and in some cases, preventing implantation. There are two main types: hormonal and copper, and understanding the differences is key.
Hormonal IUDs – like Mirena, Kyleena, Liletta, and Skyla – release a small amount of progestin, a hormone similar to the one found in birth control pills. This thins the uterine lining, making it harder for sperm to reach an egg and for a fertilized egg to implant. A major benefit is often lighter, less painful periods, sometimes even stopping periods altogether. Kyleena, for example, is known for potentially lighter bleeding than Mirena, and is approved for up to five years of use.
Copper IUDs, like Paragard, are hormone-free. They work by releasing copper ions, which are toxic to sperm, preventing fertilization. They can be used for up to 10 years, making them a really long-lasting option. However, they can sometimes cause heavier, more painful periods – something to seriously consider. Insertion can be uncomfortable, described by many as cramping, but pain management options are available, and it's usually quick.
Who's a good candidate? Hormonal IUDs are often a good fit for those wanting to lighten or stop their periods, while copper IUDs are ideal for those who prefer a hormone-free option. However, those with heavy, prolonged periods might want to avoid the copper IUD, and people with certain uterine abnormalities might not be suitable for either type. Always discuss your medical history with your doctor.
Implant Insights: A Tiny Stick, Big Impact
The Nexplanon implant is a small, flexible rod inserted under the skin of your upper arm by a healthcare provider. It releases progestin, similar to hormonal IUDs, preventing pregnancy for up to three years. It’s over 99% effective, making it one of the most reliable methods available.
Insertion involves a quick, minor procedure involving a small incision and insertion of the rod. Removal is equally straightforward. You might experience some bruising or soreness at the insertion site, but it usually resolves quickly. The biggest side effect reported is irregular bleeding, especially in the first few months. It doesn’t protect against sexually transmitted infections, so safe sex practices are still important.
Nexplanon is incredibly convenient – once it's in, you don't have to think about it for three years. However, it's not for everyone. Those sensitive to hormonal changes or who experience significant mood swings might want to explore other options. It's also important to discuss any pre-existing medical conditions with your doctor.
The Shot: Depo-Provera – Pros and Cons
Depo-Provera is an injectable contraceptive containing progestin. It’s administered by a healthcare provider every three months. It’s highly effective, but it comes with some potential side effects that need careful consideration.
The most common side effects include irregular bleeding, weight gain, and potential bone density loss. The bone density loss is reversible once you stop getting the shots, but it’s something to discuss with your doctor, especially if you have risk factors for osteoporosis. It can also take several months, even up to a year, for your fertility to return after stopping Depo-Provera.
While Depo-Provera is effective and convenient for some, it's not a one-size-fits-all solution. It’s important to be aware of the potential for weight gain and bone density loss, and to discuss these risks with your healthcare provider. It can also cause changes to your menstrual cycle, which can be unpredictable.
Permanent Options: Tubal Ligation & Essure (and its Legacy)
For those certain they don't want children, permanent contraception is an option. Tubal ligation, often called 'getting your tubes tied,' is a surgical procedure that involves blocking or removing the fallopian tubes, preventing eggs from reaching the uterus. It’s a highly effective method, but it’s permanent.
The procedure can be performed laparoscopically, meaning through small incisions, or during a C-section. Recovery typically takes a few days to a week. It's crucial to understand that tubal ligation is very difficult and expensive to reverse, so it should be considered a final decision.
Essure, a non-surgical sterilization procedure, is no longer available. It involved inserting small coils into the fallopian tubes to block them. However, it was associated with significant complications and negative experiences for many women, leading to its removal from the market. This highlights the importance of thoroughly researching any medical procedure and understanding the potential risks.
Effectiveness Compared: A Head-to-Head Look
When it comes to birth control, effectiveness rates are crucial. The CDC and FDA provide data on both 'perfect use' and 'typical use.' Perfect use refers to the method being used consistently and correctly, while typical use reflects real-world scenarios, including human error. Long-acting reversible contraceptives (LARCs) – IUDs and the implant – consistently rank highest in effectiveness.
Here's a quick comparison (based on CDC data): IUDs (hormonal & copper) and the implant have a failure rate of less than 1% with typical use. The shot (Depo-Provera) has a failure rate of around 4%. The pill, patch, and ring have failure rates around 7% with typical use, and condoms around 13%. These numbers aren't about blame; they're about understanding the margin for error.
A 'failure' doesn't always mean pregnancy. It could mean a missed shot, an expired patch, or inconsistent condom use. Having a backup plan – like condoms – is always a good idea, especially during the first few months of starting a new method, or if you're concerned about STIs. Understanding these rates helps you choose a method that aligns with your comfort level and lifestyle.
Long-Acting Reversible Contraception (LARC) Comparison for Childfree Women - 2026
| Method | Effectiveness | Hormonal Status | Reversibility | Considerations |
|---|---|---|---|---|
| IUD (Hormonal - Levonorgestrel) | Very High | Progestin-releasing | Quick, typically within days of removal | May reduce menstrual bleeding; potential for irregular spotting initially. |
| IUD (Copper) | Very High | Non-Hormonal | Quick, typically within days of removal | May cause heavier, longer periods and increased cramping. |
| Implant (Progestin) | Very High | Progestin-releasing | Quick, requires a minor in-office procedure for removal | Can cause irregular bleeding patterns; may affect mood in some individuals. |
| Sterilization (Tubal Ligation/Closure) | Very High | Non-Hormonal | Generally considered permanent, reversal is complex and not always successful | Surgical procedure; requires careful consideration due to permanence. |
| Vasal Gel (Experimental) | Potentially High | Non-Hormonal | Potentially Reversible (research ongoing) | Currently investigational; not yet widely available. Works by blocking sperm flow. |
| Birth Control Shot (Depo-Provera) | High | Progestin-releasing | Moderate - fertility returns after stopping, but can take several months | Requires injections every three months; potential for weight gain and bone density changes. |
Qualitative comparison based on the article research brief. Confirm current product details in the official docs before making implementation choices.
Cost & Coverage: What Will It *Actually* Cost?
The cost of long-term contraception varies significantly depending on the method, your insurance coverage, and your location. Generally, IUDs and the implant have a higher upfront cost – ranging from $300 to $1,300 for the device and insertion – but they’re cost-effective over time. The shot (Depo-Provera) is typically the least expensive upfront, around $0-$150 per shot, but the costs add up over time.
The Affordable Care Act (ACA) mandates that most insurance plans cover preventive services, including contraception, without cost-sharing. This means your IUD, implant, or shot should be fully covered by your insurance if you have a qualifying plan. However, you may still be responsible for consultation fees or follow-up appointments. Medicaid coverage varies by state.
Resources like Planned Parenthood and local health departments often offer affordable contraception options. You can also check with your insurance provider to understand your specific coverage and out-of-pocket expenses. Don't hesitate to ask your healthcare provider about financial assistance programs or payment plans.
Post-Procedure Comfort: Essential Items for Your Long-Term Contraception Journey

Generous 24x12 inch size for versatile use · Offers both dry and moist heat options · Features an auto shut-off for safety
This heating pad offers soothing relief for aches and pains that might accompany some long-term contraception methods.

Formulated with botanical ingredients like Arnica and MSM · Lightweight and fast-absorbing for everyday use · Non-greasy with a light, pleasant scent
Penetrex cream can help alleviate any muscle soreness or discomfort you might experience.

Designed for heavy flow with leakproof technology · Seamless construction for comfort · OEKO-TEX STANDARD 100 certified for safety
These period underwear provide reliable protection and comfort, especially during your cycle, which can sometimes be affected by contraception.

Gentle, pH-balanced formula · Specifically designed for feminine hygiene · Effectively removes odor
Summer's Eve wash offers gentle care to help you feel fresh and confident.
As an Amazon Associate I earn from qualifying purchases. Prices may vary.
Community Voices: Real Experiences
Hearing from others who have navigated these choices can be incredibly valuable. One woman in our community shared, "I chose the hormonal IUD after years on the pill, and it was a game-changer. No more daily reminders, and my periods are so much lighter."
Another member said, "I went with the copper IUD because I didn’t want hormones in my body. The heavier periods were a bit rough at first, but I adjusted, and I love the peace of mind knowing it’s hormone-free.’ A third shared, ‘Nexplanon was perfect for me. I wanted something reliable and low-maintenance, and it delivered."
These experiences highlight the diversity of preferences and needs within the childfree community. What works for one person might not work for another. The key is to do your research, talk to your healthcare provider, and choose a method that feels right for you. Remember, you're not alone in this journey.



No comments yet. Be the first to share your thoughts!