Long-term contraception options
Choosing to live childfree means you need birth control that works for years, not just until your next prescription refill. You want something reliable that doesn't require a daily thought or a trip to the pharmacy every month. Long-term options provide that security without the constant maintenance of traditional methods.
Many of us prioritize convenience, reduced anxiety, and frankly, cost-effectiveness when it comes to birth control. Constantly refilling prescriptions, remembering daily pills, or interrupting intimacy just isn't ideal. Long-acting reversible contraception (LARC) offers a 'set it and forget it' approach that minimizes user error and provides years of reliable protection. We’re going to focus on those options.
The most effective options in 2026 range from reversible inserts like IUDs and implants to permanent surgical sterilization. Each has different side effects and lifespans, so the right choice depends on how your body reacts to hormones and how permanent you want the solution to be.
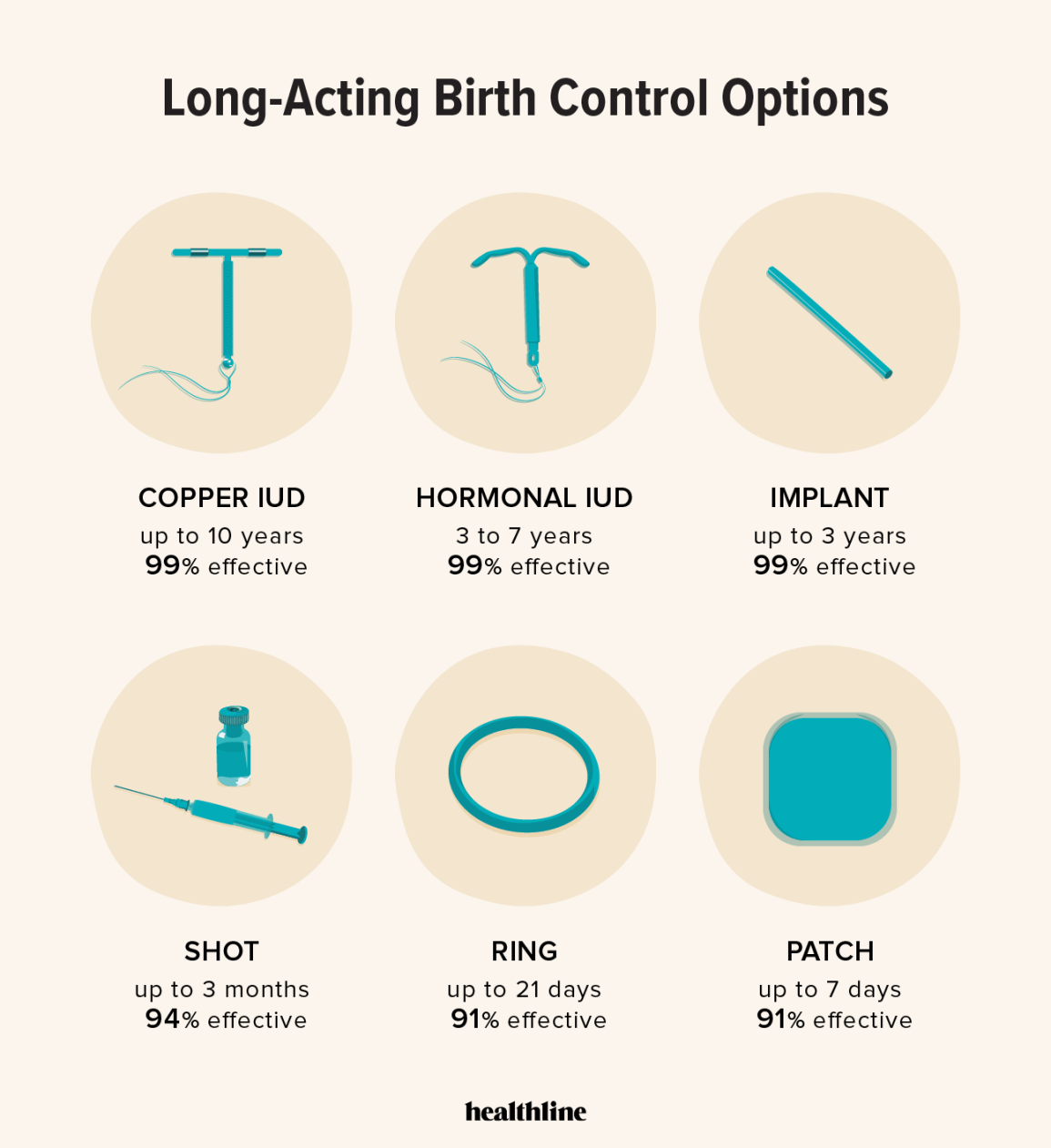
Hormonal and copper IUDs
Intrauterine Devices, or IUDs, are tiny, T-shaped devices inserted into the uterus to prevent pregnancy. They work by either preventing fertilization or, in the case of copper IUDs, creating an environment inhospitable to sperm. Insertion is typically done in a doctor’s office and, while many women report discomfort or cramping, it’s usually manageable. Expect it to feel like a strong menstrual cramp, and discuss pain management options with your provider.
There are two main types of IUDs: hormonal and copper. Hormonal IUDs – like Mirena, Kyleena, Liletta, and Skyla – release progestin, a synthetic form of progesterone. These can lighten periods, reduce cramping, and some are approved for treating heavy bleeding. They last between 3 and 8 years, depending on the brand. The copper IUD, Paragard, is hormone-free and can remain in place for up to 10 years. It’s a good option for those who prefer to avoid hormonal birth control.
IUDs are over 99% effective. According to the CDC, fewer than 1 in 100 users get pregnant annually. There are risks, though. The device can slip out of place, known as expulsion, or in rare cases, puncture the uterine wall. You'll need occasional checks to ensure it stays seated correctly.
A persistent fear surrounding IUDs is that they’ll impact fertility. This is largely a myth. Fertility returns quickly after removal for most women, often within a few cycles. However, it’s important to note that IUD insertion can rarely lead to pelvic inflammatory disease (PID), which could affect future fertility, though this is uncommon with proper screening and insertion techniques.
The contraceptive implant
The Nexplanon implant is a small, flexible rod inserted under the skin of your upper arm. It releases progestin, similar to hormonal IUDs, and prevents pregnancy for up to three years. Insertion is a quick in-office procedure, usually taking less than a minute, but local anesthesia is used to minimize discomfort. You’ll feel a small bump under your skin, but it shouldn’t interfere with daily activities.
Nexplanon is remarkably effective – even more so than IUDs, with a failure rate of less than 0.05% per year. The main side effect is irregular bleeding, which is very common, especially in the first few months. Some women experience prolonged bleeding, spotting, or no periods at all. Other potential side effects include mood changes, headaches, and weight gain, though these are less frequent.
Compared to IUDs, the implant offers convenience – no need for regular check-ups beyond annual exams. However, the unpredictable bleeding can be a dealbreaker for some. Removal is also relatively straightforward, but it can sometimes take a few minutes and may cause slight discomfort. Cycles can take several months to regulate after removal.
The implant is reversible, though your hormones might take a few months to level out after it's removed. Like all hormonal methods, it does nothing to stop sexually transmitted infections.
Long-Acting Reversible Contraception (LARC) Comparison for Childfree Women - 2026
| Method | Effectiveness | Hormonal Impact | Practical Considerations | Potential Drawbacks |
|---|---|---|---|---|
| Hormonal IUD | Very High | Present - Progestin only | Suitable for women with heavier periods; can reduce cramping. | Possible mood changes; irregular bleeding initially, potential for ovarian cysts (rare). |
| Copper IUD | Very High | Hormone-Free | Excellent for those wanting non-hormonal options; can be used as emergency contraception. | May cause heavier, longer, and more painful periods; potential for expulsion. |
| Implant | Very High | Present - Progestin only | Highly effective and discreet; lasts for several years. | Irregular bleeding is common; possible weight gain, mood changes, and headaches. |
| Combined Oral Contraceptives (Pills) | High (with perfect use) | Present - Estrogen & Progestin | Can regulate cycles and reduce acne; widely available. | Requires daily adherence; no STI protection; potential for blood clots. |
| Contraceptive Patch | High (with perfect use) | Present - Estrogen & Progestin | Convenient weekly application; more consistent hormone levels than pills. | Skin irritation possible; no STI protection; may be less effective in heavier women. |
| Contraceptive Ring | High (with perfect use) | Present - Estrogen & Progestin | Monthly insertion; lower systemic hormone exposure than pills. | No STI protection; possible vaginal irritation. |
Qualitative comparison based on the article research brief. Confirm current product details in the official docs before making implementation choices.
Pills, patches, and rings
The combined pill, patch, and vaginal ring are all effective forms of hormonal birth control, but they rely heavily on consistent and correct use. They work by releasing hormones that prevent ovulation. While they offer benefits like cycle control and potential acne improvement, their effectiveness drops significantly with even minor lapses in adherence. This makes them less ideal for long-term, low-maintenance contraception.
The typical use failure rate for the pill is around 7%, meaning 7 out of 100 women will get pregnant while using it as directed. With typical use, the patch and ring have similar failure rates. This is significantly higher than the rates associated with IUDs and implants. Life happens. We forget pills, patches fall off, and rings can be uncomfortable. These methods require diligent effort.
If you prioritize cycle control or have specific health conditions that make hormonal IUDs or the implant unsuitable, the pill, patch, or ring might be a reasonable choice. However, for those seeking the most reliable, 'set-it-and-forget-it' protection for a long-term childfree life, LARC methods are generally the superior option.
Permanent sterilization
Tubal ligation, often called 'getting your tubes tied,' is a surgical procedure that involves blocking or removing the fallopian tubes, preventing eggs from reaching the uterus. For partners with testes, a vasectomy blocks the vas deferens, preventing sperm from being released in semen. These are both considered permanent forms of birth control and should only be considered after careful thought and discussion.
Both procedures are generally safe and effective, but they are not without risks. Tubal ligation carries the risks associated with any surgery, such as infection and bleeding. Vasectomy is typically less invasive and has a quicker recovery time. Regret rates are relatively low, but they do exist – roughly 6% of women and 10% of men who undergo sterilization express regret later in life, according to a 2014 study in the Journal of the American Medical Association.
It’s crucial to remember that sterilization is not easily reversible. While tubal reversal surgery is possible, it’s not always successful. Vasectomy reversal is more often successful, but it’s still not guaranteed. Thorough counseling is essential before proceeding with either procedure. Resources like the American College of Obstetricians and Gynecologists (ACOG) and the American Urological Association (AUA) can help you find qualified surgeons and counseling services.
Cost and insurance access
The cost of long-term contraception varies depending on the method and your insurance coverage. IUDs can range from $300 to $1,000 for the device alone, while the Nexplanon implant typically costs around $1,000 to $1,500, including insertion. These costs don't include the initial consultation or follow-up visits.
Fortunately, the Affordable Care Act (ACA) generally requires most insurance plans to cover preventative care, including contraception, without cost-sharing. However, this coverage is not guaranteed for all plans, and there have been ongoing legal challenges to the ACA. Check with your insurance provider to confirm your coverage.
If you lack insurance or have high out-of-pocket costs, resources are available. Planned Parenthood and Title X clinics offer affordable or free reproductive health services, including contraception. State and local health departments may also offer assistance programs. Don't let financial barriers prevent you from accessing the birth control you need.
Comfort and Recovery Essentials for IUD and Implant Insertion

Provides moist or dry heat therapy · Features an auto-shutoff function for safety · Generously sized at 24x12 inches for broad coverage
This heating pad can offer targeted relief for potential discomfort or cramping following certain long-term contraception insertion procedures.

Contains 500 tablets of Ibuprofen · Provides anti-inflammatory and pain relief · Suitable for managing mild to moderate pain
Ibuprofen is a common over-the-counter pain reliever that can be effective in managing post-procedure discomfort.

Contains 200 Acetaminophen caplets · Offers extra strength pain relief · Each caplet contains 500 mg of Acetaminophen
Acetaminophen is an alternative pain reliever that can be used to manage discomfort after contraception insertion.

Designed for heavy flow menstrual periods · Features leakproof technology · Made with OEKO-TEX STANDARD 100 certified materials
These period underwear offer a comfortable and reliable solution for managing menstruation, which may be a consideration alongside long-term contraception.

Glare-free display for comfortable reading · Long battery life · Stores thousands of books
An e-reader can provide a welcome distraction and a sense of normalcy during recovery periods, allowing for engagement with personal interests.
As an Amazon Associate I earn from qualifying purchases. Prices may vary.



No comments yet. Be the first to share your thoughts!