Your Body, Your Choice: Contraception in 2026
Choosing whether or not to have children is a deeply personal decision. For many, contraception is a vital part of life. It’s about more than just preventing pregnancy – it’s about planning for the future you want, maintaining peace of mind in relationships, and having control over your own body and reproductive health. Prioritizing your own life and goals is valid, and effective contraception is a tool in doing so.
Contraceptive options are constantly evolving. Advancements include long-acting methods, more user-friendly hormonal options, and a growing emphasis on non-hormonal alternatives. This means there’s likely a method that fits your body, lifestyle, and preferences. Finding what empowers you to live your life, free from worry, is the goal.
This is about being informed and proactive. Whether you’re seeking temporary protection or considering a more permanent solution, understanding your options is the first step.

The Long-Acting Powerhouses: IUDs & Implants
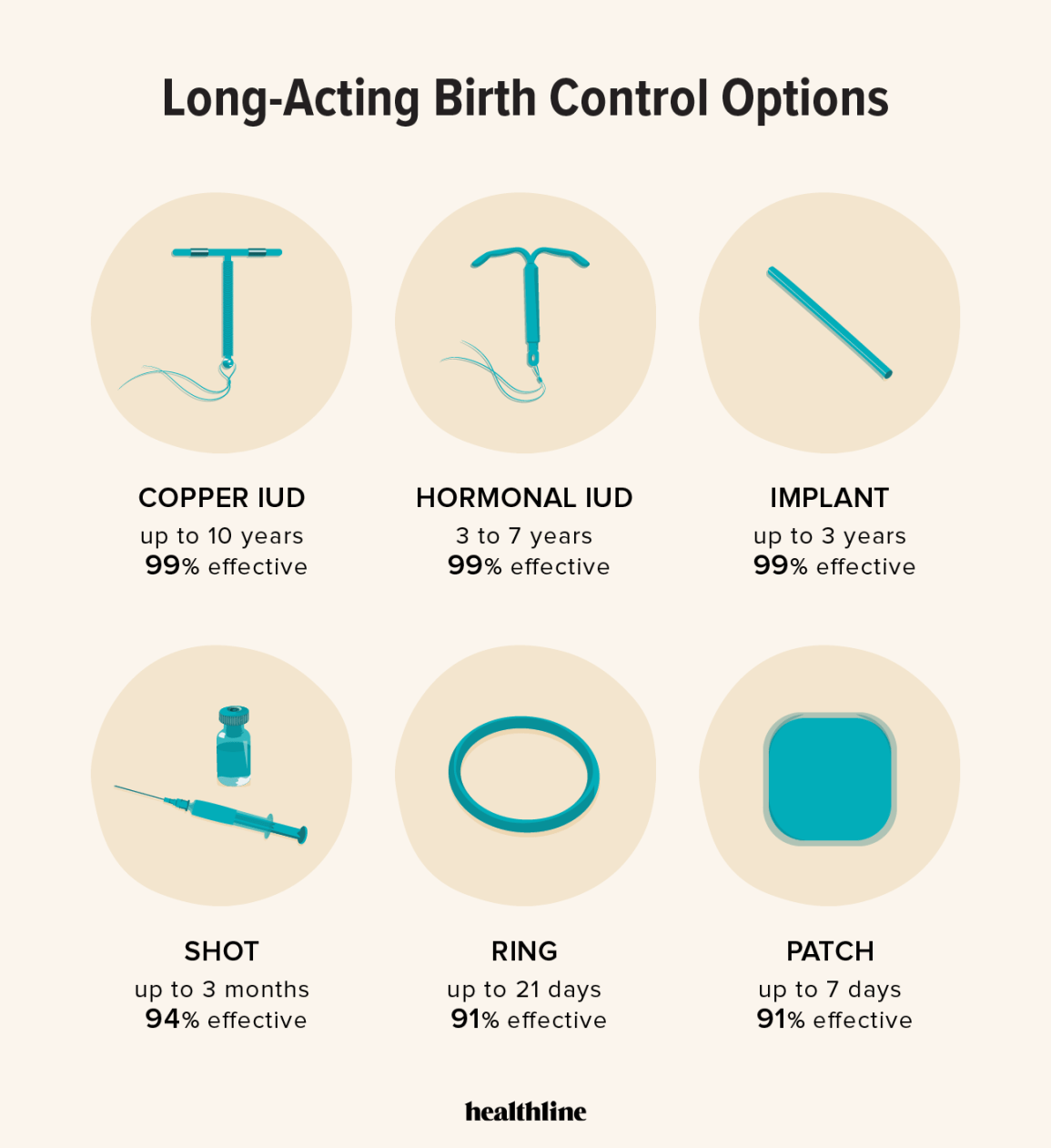
Long-Acting Reversible Contraception (LARC) offers reliable protection for years. This category includes hormonal IUDs like Mirena, Kyleena, Liletta, and Skyla, the copper IUD (Paragard), and the implant, Nexplanon. These methods are effective because you don't have to remember to do anything after they're in place.
Hormonal IUDs release progestin, a synthetic form of progesterone, into the uterus. This thickens cervical mucus, making it difficult for sperm to reach the egg, and can also thin the uterine lining. The copper IUD, on the other hand, doesn’t use hormones. It creates an inflammatory response that is toxic to sperm. According to the CDC, IUDs are over 99% effective. The implant, a small rod inserted under the skin of your upper arm, releases progestin and is also over 99% effective.
Insertion is often described as cramping, and experiences vary. Some people find it quick and relatively painless, while others experience more discomfort. Pain management options, like over-the-counter pain relievers or local anesthesia, are available and should be discussed with your healthcare provider. Potential side effects of hormonal IUDs can include irregular bleeding, spotting, and hormonal fluctuations. The copper IUD can sometimes lead to heavier periods, and the implant can cause irregular bleeding patterns.
These methods are suitable for people who want set-it-and-forget-it contraception. They're also reversible – when removed, fertility typically returns quickly. Costs vary depending on insurance coverage, but typically range from $0-$1300 upfront for the device, plus the cost of the insertion appointment. Many insurance plans now cover LARC methods without cost-sharing due to the Affordable Care Act.
- Mirena: Effective for up to 8 years.
- Kyleena: Effective for up to 5 years.
- Liletta: Effective for up to 8 years.
- Skyla: Effective for up to 3 years.
- Paragard: Effective for up to 10 years.
- Nexplanon: Effective for up to 3 years.
IUD vs. Implant: A Comparison for the Childfree Lifestyle (2026)
| Feature | Hormonal IUD | Copper IUD | Implant |
|---|---|---|---|
| Hormone-Free Option | No | Yes | No |
| Duration of Effectiveness | 3-8 years | Up to 10 years | 3 years |
| Ease of Removal | Moderate - Requires healthcare provider | Moderate - Requires healthcare provider | Moderate - Requires healthcare provider, may be more complex than IUD removal |
| Potential Side Effects | Possible irregular bleeding, hormonal side effects | Possible heavier/longer periods, cramping | Possible irregular bleeding, hormonal side effects (mood changes, weight fluctuations) |
| Upfront Cost | Moderate to High (includes consultation & insertion) | Moderate to High (includes consultation & insertion) | Moderate to High (includes consultation & insertion) |
| Ongoing Costs | Low - Routine checkups only | Low - Routine checkups only | Low - Routine checkups only |
| Suitability - Medical History | Generally suitable, but consider hormone sensitivities/history of uterine issues | Good option for those avoiding hormones, but may not be suitable for those with heavy bleeding or copper allergies | Generally suitable, but consider hormone sensitivities/history of migraines or blood clots |
Illustrative comparison based on the article research brief. Verify current pricing, limits, and product details in the official docs before relying on it.
Hormonal Methods: Beyond the Pill
Beyond IUDs and implants, other hormonal options are available. The traditional birth control pill remains a common choice, with various formulations of estrogen and progestin. The patch, Xulane, is a transdermal patch applied weekly, and the ring, NuvaRing, is inserted into the vagina monthly. These methods release hormones to prevent ovulation.
The pill requires daily adherence, which can be a drawback. The patch and ring offer more convenience, requiring less frequent attention. All three methods rely on consistent use to maintain their effectiveness – around 91% with typical use. Potential side effects are similar to hormonal IUDs: mood changes, weight fluctuations, and irregular bleeding are possible, though experiences vary.
Newer pill formulations focus on minimizing side effects or offering more consistent hormone levels. Research into how different progestins impact mood suggests some formulations are less likely to cause mood swings. Discuss your individual health history and concerns with your doctor to find the best option. What works for one person may not work for another.
Concerns exist about the impact of hormonal birth control on mood and weight. While some people experience these side effects, many do not. Correlation doesn’t equal causation, and other factors can play a role in mood and weight changes.
Barrier Methods: Control and Protection
Barrier methods physically block sperm from reaching the egg. This category includes male condoms, female condoms, diaphragms, cervical caps, and spermicides. Male condoms are the most widely used barrier method, offering around 85% effectiveness with typical use. Female condoms are less common but offer a user-controlled option.
Diaphragms and cervical caps are reusable silicone cups inserted into the vagina before intercourse and used with spermicide. They require a prescription and proper fitting by a healthcare provider. Spermicides alone are not very effective, but can be used with other barrier methods to increase protection.
A significant advantage of barrier methods is that they also protect against sexually transmitted infections (STIs). This is a major benefit, especially if you have multiple partners or are unsure of your partner’s STI status. While they require more conscious effort than other methods, they offer a non-hormonal option for those who prefer to avoid hormonal contraception.
undefined for a more environmentally friendly approach.
Permanent Options: Sterilization for the Certain
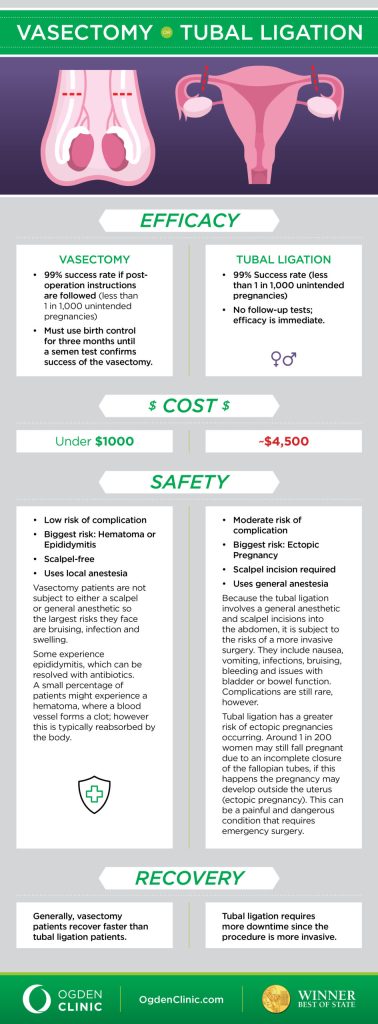
For those who are absolutely certain they do not want to have children, sterilization offers a permanent solution. For partners with testes, a vasectomy involves cutting or blocking the vas deferens, preventing sperm from being released in semen. For those with a uterus, tubal ligation involves blocking or removing the fallopian tubes, preventing the egg from traveling to the uterus. Increasingly, doctors are performing salpingectomies – removing the fallopian tubes entirely – which also reduces the risk of certain types of ovarian cancer.
Vasectomies are typically performed in a doctor’s office under local anesthesia and have a relatively quick recovery time. Tubal ligation is usually performed laparoscopically, requiring a slightly longer recovery period. It's vital to understand that sterilization is considered permanent, although reversal surgery is sometimes possible, it’s not always successful.
Thorough counseling is essential before undergoing sterilization. Healthcare providers should discuss the permanence of the procedure, potential risks and benefits, and alternative contraception options. It’s crucial to be absolutely certain about your decision, as reversing the procedure can be costly, complicated, and not always effective.
Common anxieties around sterilization often involve concerns about sexual function or regret. However, studies have shown that sterilization does not typically affect sexual desire or performance. The increasing trend of tubal removal as a cancer prevention measure is also influencing more people to consider this permanent option.
Emergency Contraception: A Safety Net
Emergency contraception (EC) is a backup option to prevent pregnancy after unprotected sex or contraceptive failure. The most effective form of EC is inserting a copper IUD within five days of unprotected sex. EC pills are also available in two types: levonorgestrel pills (like Plan B One-Step) and ulipristal acetate pills (like ella).
Levonorgestrel pills are available over-the-counter and work by delaying ovulation. Ulipristal acetate pills require a prescription and are more effective, especially if you’re closer to ovulation. It’s important to use EC as soon as possible after unprotected sex for maximum effectiveness. EC is not the same as an abortion pill and will not terminate an existing pregnancy.
Accessing EC discreetly is often a concern. Many pharmacies carry levonorgestrel pills over-the-counter, and telehealth services can provide prescriptions for ulipristal acetate pills. Knowing your options and having a plan in place can provide peace of mind.
There are many myths surrounding EC. It’s important to rely on accurate information from trusted sources. EC is a safe and effective way to prevent unintended pregnancy when used correctly.
Worth a Closer Look: Emerging Technologies
The field of contraception is continually evolving. Researchers are exploring new non-hormonal options, including gels and spermicides that target sperm motility. There’s also ongoing research into new delivery methods for existing hormones, aiming for more consistent and convenient administration. Perhaps the most exciting area of development is male contraception – with several methods in clinical trials, ranging from gels to injections.
However, it's important to be cautious about overhyping these technologies. Many are still in the early stages of development and may not be widely available for several years. It’s best to view these as 'what’s on the horizon' rather than immediate solutions. Staying informed about the latest research can help you make informed decisions when new options become available.
The focus on non-hormonal options is particularly encouraging for those who experience side effects from hormonal birth control. A wider range of choices will ultimately empower individuals to find the method that best suits their needs and preferences.
Finding the Right Fit: Resources & Support
Navigating the world of contraception can feel overwhelming, but you don’t have to do it alone. Planned Parenthood () offers comprehensive reproductive health services, including contraception counseling and access. Bedsider () is a great online resource with unbiased information about all contraceptive methods.
The CDC () provides evidence-based guidance for healthcare providers and the public. If you’re struggling to afford contraception, explore financial assistance programs offered by organizations like Planned Parenthood and local health departments.
Remember, taking control of your reproductive health is empowering. There’s a contraception method out there for everyone, and finding the right fit is an investment in your future. Don’t hesitate to talk to your healthcare provider, do your research, and advocate for your own needs.
Your Childfree Toolkit: Essential Comforts for Your Birth Control Journey

Focuses on home organization and lifestyle tips · Features a 'Tick A Pantry Off Your Wish List' segment
While not a direct contraception method, this magazine can inspire a sense of order and control in your living space, aligning with a planned lifestyle.

Water-based lubricant · Paraben-free formula · 8oz bottle
Enhances comfort and pleasure during intimacy, making sexual health practices more enjoyable and accessible.

Reusable period underwear · Absorbs up to 12 regular tampons' worth of flow · Leakproof and odor-controlling technology
Offers a comfortable and sustainable alternative for managing periods, reducing waste and providing peace of mind.

Extra-large electric heating pad · Designed for full-body pain relief, including menstrual cramps · Features 6 heat settings and 4 timer options
Provides targeted relief for menstrual discomfort, promoting comfort and well-being during your cycle.
As an Amazon Associate I earn from qualifying purchases. Prices may vary.



No comments yet. Be the first to share your thoughts!