Permanent Choices: A 2026 Overview
Deciding whether or not to have children is deeply personal, and choosing permanent birth control is a significant step. It's okay to feel a lot of different emotions as you consider your options. This guide offers clear, honest information about sterilization procedures as they stand in 2026, without judgment. We’ll explore the most common methods – vasectomy and tubal ligation – as well as some less frequently used alternatives.
Reproductive autonomy is increasingly recognized as a fundamental right, and making an informed decision requires access to accurate information. The procedures available, and even access to those procedures, can vary depending on where you live, so we’ll provide a broad overview and resources for finding care. You deserve to feel empowered and confident in your choice, whatever that may be.
We’ll cover what each procedure entails, the recovery process, potential risks, and the financial aspects. This guide aims to give you the tools to have a productive conversation with your healthcare provider and make the best decision for your life.
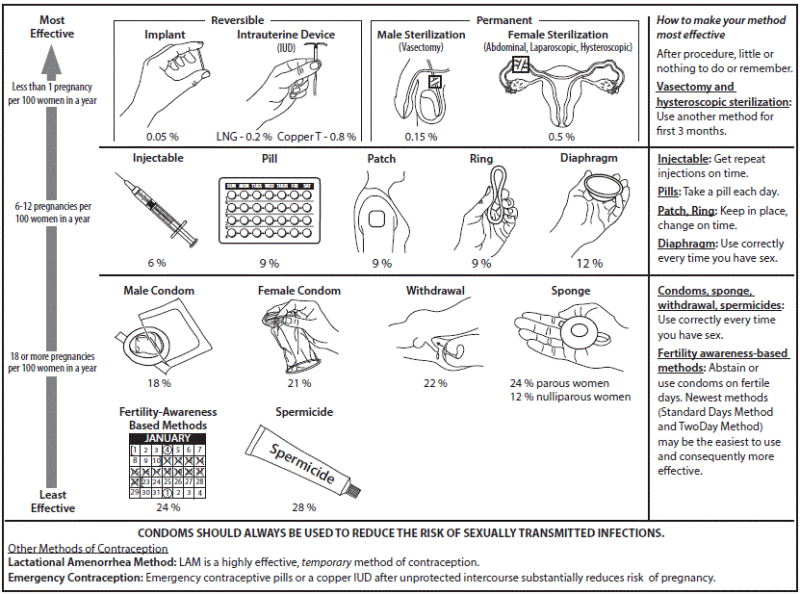
You don’t know how to prevent pregnancy? Spare me. He can cover it or you have multiple options the pill a diaphragm a tubal ligation and plan B. Plus abortion up to 13 weeks depending on your state.
— LadyMary (@JaneRiordan) May 4, 2026
Vasectomy: Details & Recovery
A vasectomy is a surgical procedure for male sterilization, blocking sperm from reaching the semen. It’s generally considered a simpler and less invasive procedure than tubal ligation. During the surgery, the vas deferens—the tubes that carry sperm—are cut, sealed, or blocked. This prevents sperm from mixing with the semen during ejaculation.
There are two main techniques: the traditional vasectomy, which involves one or two small incisions in the scrotum, and the no-scalpel vasectomy, which uses a small puncture to access the vas deferens. The no-scalpel method often results in less pain and quicker recovery. Most vasectomies are performed in an outpatient setting, meaning you go home the same day.
Pain levels vary, but most men report discomfort rather than severe pain. Over-the-counter pain relievers are usually sufficient. You’ll likely experience some swelling and bruising, which typically subsides within a week or two. Avoid strenuous activity for a week or so after the procedure. While many men feel back to normal quickly, it takes time for the body to clear existing sperm.
You’ll need to provide semen samples after the vasectomy to confirm that no sperm are present. This usually involves several tests over a few months. A small number of sperm may still be present initially, and follow-up testing is essential. While vasectomies are highly effective, they aren’t 100% foolproof. Rare complications can include infection, bleeding, or chronic pain. The American Urological Association reports a complication rate of less than 1%.
Vasectomy reversal is an option, but it’s not always successful. Success rates depend on several factors, including the time since the vasectomy and the technique used for the reversal. The cost of a reversal can be substantial, ranging from $3,000 to $10,000 or more according to the Mayo Clinic.
- Consultation with a urologist to discuss the procedure and address any concerns.
- The vasectomy procedure itself, typically taking 20-30 minutes.
- Post-operative care, including rest, ice packs, and pain management.
- Semen analysis to confirm sterility.
Tubal Ligation: Options Explained
Tubal ligation, often called getting your "tubes tied,’ is a surgical procedure for female sterilization. It involves blocking or removing the fallopian tubes, preventing eggs from traveling to the uterus. There are several methods for achieving this, each with its own pros and cons. The choice of method often depends on the individual’s circumstances and the surgeon"s preference.
Common methods include burning (cauterization), clipping, banding, and removal of the tubes (salpingectomy). Cauterization uses heat to seal the tubes, while clipping involves applying small clamps. Banding uses a small band to tie off the tubes. Salpingectomy, the removal of the tubes, is becoming increasingly recommended, as it also reduces the risk of ovarian cancer, according to a 2017 study published in The Lancet.
Tubal ligation is usually performed laparoscopically, meaning small incisions are made in the abdomen and a camera and surgical instruments are used to access the fallopian tubes. It can also be performed postpartum, shortly after childbirth. Laparoscopic surgery generally results in a faster recovery than traditional open surgery, but it still requires some downtime.
Recovery time varies, but most women can return to normal activities within a week or two. Pain management typically involves over-the-counter pain relievers. Potential risks include infection, bleeding, and ectopic pregnancy – though the risk of ectopic pregnancy is significantly reduced with salpingectomy. Menstruation is generally not affected by tubal ligation, though some women report changes in their periods.
Reversing a tubal ligation is possible, but it’s often more difficult and expensive than reversing a vasectomy. Success rates depend on the method used for the original sterilization and the extent of damage to the fallopian tubes. Reversal surgery can cost upwards of $8,000 to $20,000, and there’s no guarantee of success. The American Society for Reproductive Medicine indicates that the success rate for tubal ligation reversal ranges from 50-80%.
Beyond the 'Standard' Options
While vasectomy and tubal ligation are the most common sterilization procedures, other options exist, though they are less frequently used. Essure, a non-surgical procedure involving the placement of small coils in the fallopian tubes, was once popular, but it has been largely discontinued due to safety concerns and numerous lawsuits. If Essure is still available in your area, it’s vital to be fully aware of the potential risks.
Hysteroscopies with tubal implants involve inserting small plugs into the fallopian tubes using a hysteroscope. This method is less invasive than traditional tubal ligation, but it's not as widely available and long-term data is limited. Salpingectomy, as mentioned earlier, is gaining traction as it offers both sterilization and a reduced risk of ovarian cancer.
These less common procedures should be discussed thoroughly with a qualified healthcare provider. It’s essential to understand the potential benefits and drawbacks, as well as the long-term implications. The best option for you will depend on your individual circumstances and preferences. Don’t hesitate to ask questions and seek a second opinion if you’re unsure.
Cost & Insurance Coverage in 2026
The cost of sterilization procedures can vary significantly depending on the location, the surgeon’s fees, facility fees, and anesthesia costs. In 2026, a vasectomy typically ranges from $500 to $2,000, while tubal ligation can cost between $2,000 and $6,000. These are just estimates, and the actual cost may be higher or lower.
Insurance coverage for sterilization procedures varies widely by plan and state. Many insurance plans cover sterilization procedures, but some may require prior authorization or have specific stipulations. The Affordable Care Act (ACA) generally requires most insurance plans to cover sterilization without cost-sharing, but there are exceptions, particularly for grandfathered plans.
Out-of-pocket expenses can include deductibles, co-pays, and co-insurance. It’s crucial to contact your insurance provider to understand your specific coverage. Resources for finding financial assistance programs include Planned Parenthood and the National Family Planning & Reproductive Health Association.
Costs are subject to change, so it’s essential to verify the information with your insurance provider and the healthcare facility before scheduling the procedure. Don’t be afraid to ask for a detailed cost estimate and explore payment options.
Comparing Permanent Sterilization Options (2026)
| Procedure | Cost | Recovery | Reversibility | Complication Risk |
|---|---|---|---|---|
| Vasectomy (for people with testes) | Generally Lower | Short (few days) | Difficult & Expensive | Low |
| Tubal Ligation (for people with a uterus and fallopian tubes) | Medium | Medium (several days to a week) | Difficult & Expensive | Medium |
| Hysterectomy (removal of the uterus) | Medium to High | Longer (several weeks) | Unlikely - eliminates future fertility | Medium to High, depends on approach |
| Salpingectomy (removal of fallopian tubes) | Medium | Medium (several days to a week) | Unlikely - permanent | Low to Medium |
| Essure (Cystourethral device - *availability varies* - check with your provider) | Medium | Short (few days) | Difficult & May Require Further Procedure | Medium |
| Bilatera Tubal Implants (RISUS) | Medium | Short (few days) | Difficult & Expensive | Low to Medium |
Qualitative comparison based on the article research brief. Confirm current product details in the official docs before making implementation choices.
Finding a Supportive Provider
Finding a healthcare provider who is respectful, informed, and non-judgmental is paramount. You deserve to feel comfortable discussing your reproductive choices without pressure or bias. Ask friends or family for recommendations, or search online directories. The American Association of Gynecologic Laparoscopists (AAGL) offers a directory of qualified laparoscopic surgeons.
When you meet with a potential provider, ask questions about their experience with sterilization procedures, their success rates, and their approach to patient care. Don’t hesitate to ask about potential risks and complications. Pay attention to how they respond to your questions and whether they seem genuinely interested in your well-being.
Unfortunately, some healthcare providers may exhibit bias or attempt to influence your decision. If you feel pressured or uncomfortable, seek a second opinion. You have the right to advocate for yourself and choose a provider who respects your autonomy. Remember, this is your body and your decision.
Emotional & Relationship Considerations
Choosing permanent birth control is a big decision with emotional weight. Acknowledge and process your feelings, whether they’re relief, sadness, or uncertainty. Even if you’re confident in your decision, it’s normal to experience a range of emotions. If you're in a relationship, open and honest communication with your partner is essential. Discuss your reasons for considering sterilization and address any concerns they may have.
Some individuals may experience feelings of grief or loss, even if they’ve always known they didn’t want children. This is a normal reaction, and you should allow yourself time to grieve. Consider seeking counseling or joining a support group to process your emotions. Self-care is also crucial during this time – prioritize activities that bring you joy and relaxation.
Post-Procedure Life: What to Expect
After sterilization, you won’t experience any significant changes in your hormone levels or overall health. Sterilization does not cause menopause or affect your libido. Continue with regular checkups and screenings. While sterilization eliminates the risk of pregnancy, it does not protect against sexually transmitted infections.
undefined, confident in your decision and empowered by your reproductive autonomy.
Remember, you’ve made a thoughtful choice about your future. Embrace your freedom and continue to prioritize your well-being. Your path is valid, and you deserve to live your best childfree life.

No comments yet. Be the first to share your thoughts!