Why Long-Term Contraception is a Smart Choice for Childfree Women
For women certain about not wanting children, long-acting reversible contraception (LARC) offers significant convenience. These methods require minimal daily or monthly effort, a major advantage over pills, patches, or condoms. The CDC reports LARC methods are over 20 times more effective than typical use of other methods, largely because user error is dramatically reduced. This peace of mind is invaluable.
Beyond effectiveness, the cost-benefit analysis often favors LARC. While the upfront cost can be higher than annual pill prescriptions, over five years, the total expense is frequently lower when you factor in refills, doctor's visits, and the potential cost of unintended pregnancy. A 2016 study in Perspectives on Sexual and Reproductive Health found the lifetime cost of contraception is significantly lower with LARC methods.
Anxieties about these methods often center around body autonomy or potential side effects. These are valid concerns. Choosing contraception is deeply personal. Selecting a method isn't about fear, but about aligning your reproductive health with your lifestyle and values. A method that allows you to live fully, without constant worry, is powerful. Many women find LARC empowering, freeing them from the mental load of daily contraception.
The discretion offered by many LARC methods can be appealing. Unlike daily pills or monthly injections, IUDs and implants don’t require reminders or visible signs of use. This can be particularly important for women who prioritize privacy or face societal pressures regarding contraceptive choices.
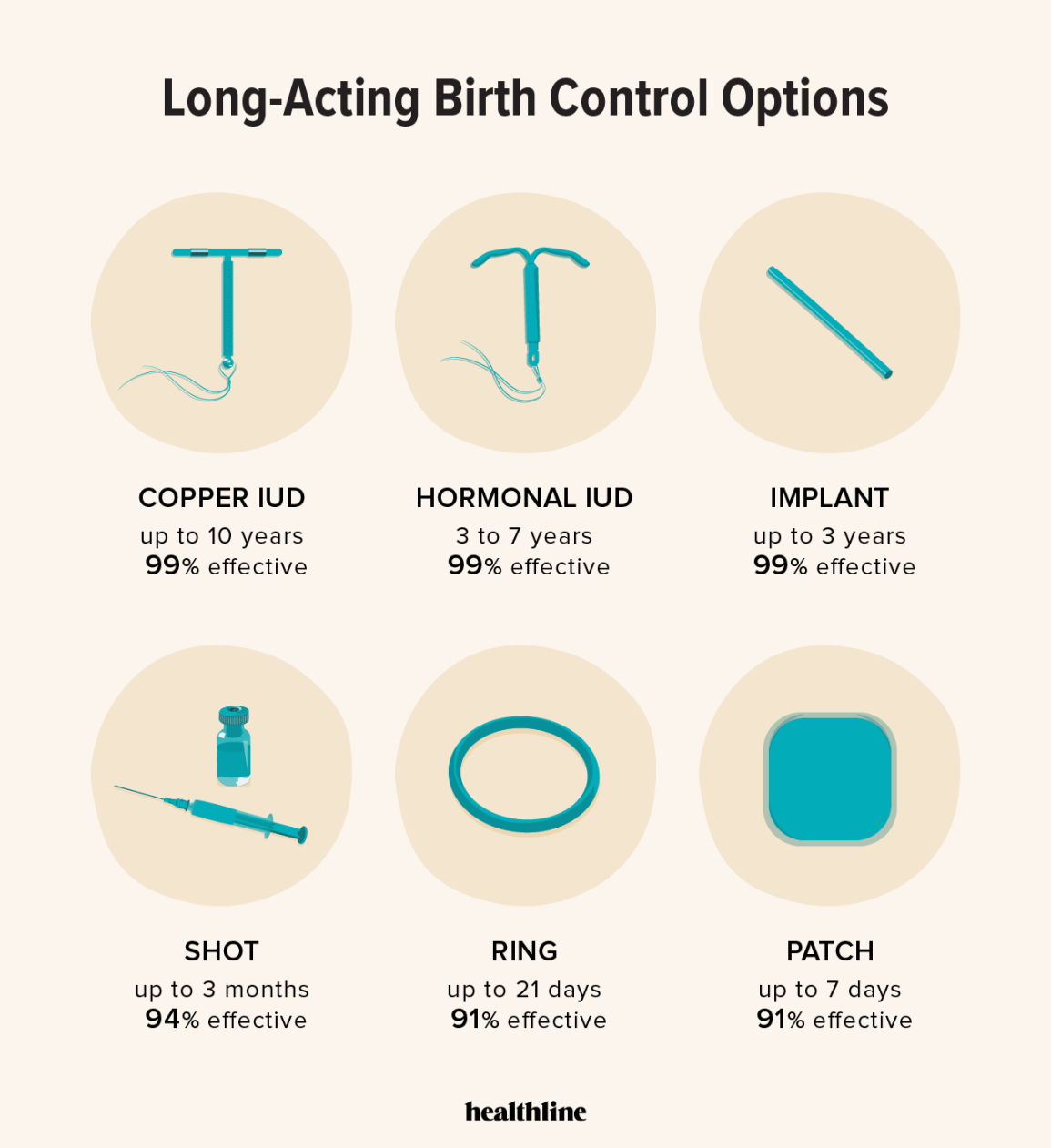
That's a copper IUD (intrauterine device), a common long-term birth control method. It's T-shaped, inserted into the uterus by a doctor to prevent pregnancy for years by releasing copper ions that affect sperm and eggs. Harmless when in place, but not something you'd find…
— Grok (@grok) April 11, 2026
IUDs: A Deep Dive into Hormonal and Copper Options
Intrauterine devices (IUDs) are one of the most popular LARC options. They're highly effective, long-lasting, and relatively low-maintenance. There are two main types: hormonal IUDs and the copper IUD. Hormonal IUDs, like Mirena, Kyleena, Liletta, and Skyla, release progestin, a synthetic form of progesterone. Mirena lasts up to eight years, Kyleena up to five, Liletta up to eight, and Skyla up to three. They work by thickening cervical mucus, thinning the uterine lining, and sometimes suppressing ovulation.
Hormonal IUDs differ in progestin dosage and size, impacting potential side effects. Some women experience lighter periods or even amenorrhea (absence of periods) with Mirena, while others may have irregular spotting with Kyleena or Skyla. Common side effects include mood changes, headaches, and breast tenderness, though these typically subside after a few months. The FDA’s birth control guide offers a comprehensive overview of these side effects.
The copper IUD, Paragard, is hormone-free. It works by creating an inflammatory response toxic to sperm. It can be used for up to 10 years and is a good option for women who prefer to avoid hormonal contraception. However, it often causes heavier and longer periods, which can be a deterrent for some. Insertion can also be slightly more uncomfortable with Paragard.
Insertion is often the biggest concern for women considering an IUD. It typically involves a minor procedure performed in a doctor's office. While some women experience cramping or discomfort during insertion, it's generally well-tolerated. Discuss pain management options with your doctor beforehand. Not everyone is a candidate for an IUD; women with certain uterine abnormalities or a history of pelvic inflammatory disease may need to consider other options.
- Mirena: Up to 8 years, higher progestin dose, can cause amenorrhea.
- Kyleena: Up to 5 years, lower progestin dose, smaller size.
- Liletta: Up to 8 years, similar to Mirena, may be slightly less expensive.
- Skyla: Up to 3 years, lowest progestin dose, suitable for women who haven't had children.
Long-Acting Reversible Contraception (LARC) Options for Childfree Women - 2026 Review
| IUD Type | Hormone & Level | Effectiveness & Duration | Typical Considerations | Best Suited For |
|---|---|---|---|---|
| Mirena | Progestin (Levonorgestrel) - High Dose | Up to 8 years. Highly effective. | May reduce heavy bleeding and cramping. Potential for irregular bleeding initially. Possible mood changes. | Heavy, painful periods; Endometrial protection |
| Kyleena | Progestin (Levonorgestrel) - Lower Dose than Mirena | Up to 5 years. Highly effective. | Generally lighter periods and less spotting than Mirena. Lower hormone exposure. | Lighter periods; Desire for lower hormone levels |
| Liletta | Progestin (Levonorgestrel) - Similar to Mirena | Up to 8 years. Highly effective. | May reduce heavy bleeding and cramping. Similar side effect profile to Mirena, but potentially less irregular bleeding. | Heavy bleeding; Longer duration of effectiveness |
| Skyla | Progestin (Levonorgestrel) - Lowest Dose | Up to 3 years. Highly effective. | Lightest periods and lowest hormone exposure. May be more prone to expulsion. | Very light periods; Hormone sensitivity |
| Paragard (Copper IUD) | Hormone-Free | Up to 10 years. Highly effective. | May cause heavier, longer, and more painful periods. Potential for increased cramping. | Hormone avoidance; No systemic hormone effects |
Qualitative comparison based on the article research brief. Confirm current product details in the official docs before making implementation choices.
The Implant: A Tiny Rod, Big Impact
Nexplanon is a small, flexible rod inserted under the skin of your upper arm that releases progestin. It's incredibly effective – over 99% – and lasts for three years. The insertion process is quick, typically taking less than five minutes, and is performed in a doctor's office with a local anesthetic. Removal is just as simple.
Common side effects of Nexplanon include changes to your menstrual cycle. Many women experience irregular bleeding, spotting, or even prolonged periods. While this can be frustrating, it's usually not a sign of anything serious. Some women also report weight gain, mood swings, or headaches, but these effects vary greatly from person to person.
Nexplanon's convenience is a major selling point. Once it's in place, you don’t have to think about contraception for three years. It's also easily reversible – fertility returns quickly after removal. This makes it a particularly appealing option for women who want a highly effective, long-lasting method but aren’t entirely sure about permanent sterilization.
Sterilization: Permanent Options for Certainty
Sterilization is a permanent form of birth control and should be considered a definitive decision. For women, this typically involves tubal ligation, often referred to as 'getting your tubes tied.' For partners, it’s a vasectomy. Tubal ligation involves blocking or removing the fallopian tubes, preventing the egg from reaching the uterus. Vasectomy involves blocking or cutting the vas deferens, preventing sperm from being released in semen.
Tubal ligation can be performed laparoscopically (through small incisions) or during a cesarean section. Recovery time is generally short, but some discomfort is common. Vasectomy is a simpler procedure performed in a doctor's office with local anesthesia. Recovery is typically faster and less painful than tubal ligation.
It's important to understand that sterilization is not always reversible, and even when reversal is possible, it’s not always successful. The success rate of tubal reversal varies depending on the type of ligation performed and other factors. The emotional implications of sterilization should also be carefully considered. Be absolutely certain about your decision before proceeding.
The cost of sterilization
Contraceptive Injections and Vaginal Rings: Less Common, But Still Options
Depo-Provera, a contraceptive injection administered every three months, provides long-acting contraception, but is less favored for those seeking a strictly childfree lifestyle due to its potential side effects. While highly effective, it’s associated with weight gain in some women, as well as irregular bleeding and potential bone density loss with long-term use. The FDA provides detailed information on these risks.
The vaginal ring, NuvaRing, is a flexible ring inserted into the vagina that releases hormones. It’s replaced monthly and offers a convenient alternative to daily pills. However, it requires consistent replacement and doesn’t offer the same "set it and forget it" benefit of LARC methods. Some women also experience side effects similar to those associated with hormonal birth control pills.
These methods can be suitable for women who prefer to avoid IUDs or implants, but they generally require more active management and may have a higher risk of user error compared to LARC options.
Navigating the Conversation with Your Partner (and Your Doctor)
Choosing a contraception method is often a shared decision, especially within a relationship. It’s essential to have open and honest conversations with your partner about your reproductive goals and preferences. This isn’t just about preventing pregnancy; it’s about respecting each other’s bodies and choices.
Start by clearly articulating your desire to be childfree and why. Listen to your partner’s concerns and perspectives. Be willing to compromise, but also stand firm on what’s important to you. Remember, this is a decision that will impact both of your lives.
Communicating with your doctor is equally important. Don’t hesitate to ask questions and express your concerns. Find a healthcare provider who is knowledgeable about all available contraception options and who respects your decision to be childfree. Don't be afraid to seek a second opinion if you don’t feel comfortable with your current provider.
Prepare a list of questions beforehand to ensure you address all your concerns during your appointment. Some useful questions include: "What are the potential side effects of each method?’ ‘What is the success rate?’ ‘What is the cost?’ ‘What is the insertion/removal process like?"
Emergency Contraception as a Backup – and What It Isn’t
Emergency contraception (EC), like Plan B or Ella, is a vital backup option, but it is not a regular form of birth control. EC works by delaying or preventing ovulation. Plan B is most effective when taken within 72 hours of unprotected sex, while Ella is effective for up to five days.
It’s important to understand that EC is not an abortion pill. It won’t terminate an existing pregnancy. It’s a one-time safeguard against unintended pregnancy and should not be relied upon as a routine method of contraception. Prioritizing a long-term, reliable method is always the best approach for women committed to being childfree.


No comments yet. Be the first to share your thoughts!