The childfree contraception foundation
The decision to live a childfree life is deeply personal, and increasingly, a valid and intentional choice for many. It’s a decision that deserves respect and, importantly, proactive planning. For those committed to remaining childfree, reliable contraception isn't about preventing something unwanted, but about maintaining a desired life state. It’s about agency and control over your reproductive future.
Often overlooked is the emotional component of contraception when a childfree life is the goal. The anxiety surrounding potential unintended pregnancy can be significant. Finding a method you trust, and that aligns with your body and lifestyle, can drastically reduce this stress. It allows you to live more fully in the present, confident in your choices.
Choosing a method for 2026 means looking at the hard data on failure rates and the reality of daily maintenance. If you're certain about not having kids, the priority shifts from temporary fixes to high-reliability systems that don't require constant attention.
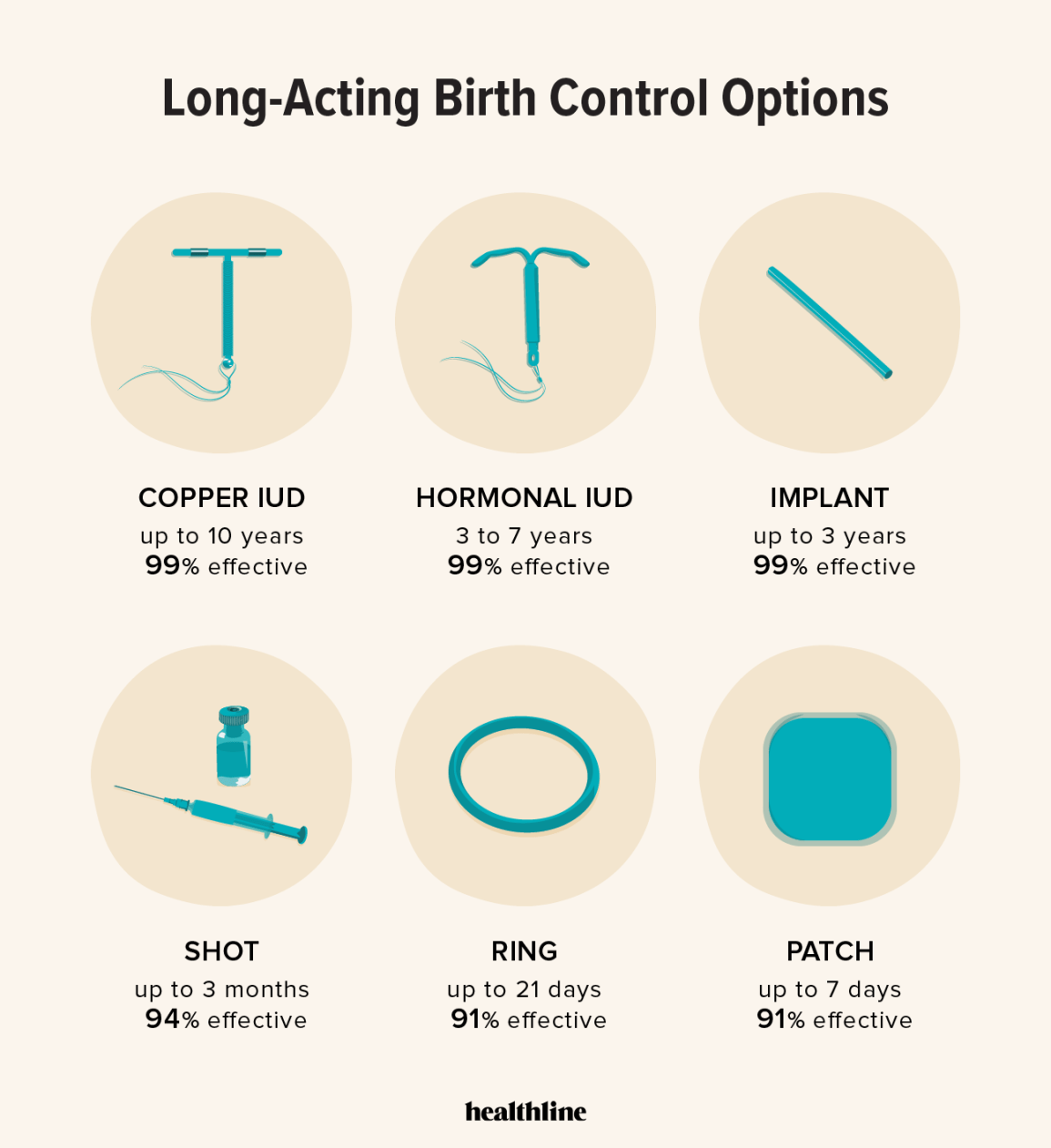
Long-acting reversible contraception
Long-Acting Reversible Contraception, or LARC, consistently ranks as the most effective form of reversible birth control. This category includes intrauterine devices (IUDs) – both hormonal and copper – and implants. These methods require minimal user intervention after insertion, significantly reducing the risk of user error.
IUDs work by changing the uterine environment or using copper to disable sperm. Hormonal versions like Mirena or Kyleena also thicken cervical mucus. CDC data from 2024 shows typical failure rates for hormonal IUDs are around 0.2%, while the copper Paragard sits at 0.8%.
Implants, such as Nexplanon, release progestin and prevent ovulation. They boast a perfect and typical use failure rate of less than 0.05%, making them exceptionally reliable. Common side effects of hormonal LARCs can include irregular bleeding, mood changes, and headaches, while the copper IUD may cause heavier periods and cramping. The initial cost of LARC methods can be higher – typically $300 to $1000 including insertion – but they offer long-term cost savings by eliminating the need for ongoing purchases.
I'll be honest, the insertion process can be daunting. Many people experience anxiety or discomfort. Pain management options, like local anesthesia or over-the-counter pain relievers, are available and should be discussed with your healthcare provider. Removal is generally simpler and less painful than insertion, but it’s still important to be prepared and informed.
Hormonal options
While the daily pill remains a popular choice, several other hormonal methods offer varying levels of convenience and consistency. These include the contraceptive patch (Xulane), the vaginal ring (NuvaRing), and the injectable contraceptive (Depo-Provera). All work primarily by releasing hormones – estrogen and/or progestin – to prevent ovulation.
The patch is applied weekly to the skin, while the ring is inserted into the vagina and replaced monthly. Depo-Provera is an injection administered every three months. These methods offer the convenience of not requiring daily attention, which can improve consistency. Effectiveness rates are comparable to the pill, around 91% with typical use, but adherence is crucial.
However, hormonal birth control isn’t a one-size-fits-all solution. Side effects vary greatly from person to person and can include mood swings, weight changes, breast tenderness, and spotting. It’s vital to discuss your medical history and any existing conditions with your doctor to determine if hormonal birth control is right for you.
Different methods use different types of hormones and dosages, impacting their effect on the menstrual cycle. Some methods may lead to lighter or absent periods, while others may cause irregular bleeding. Understanding these potential effects is crucial for making an informed decision.
Barrier methods
Barrier methods physically prevent sperm from reaching the egg. This category includes male condoms, female condoms, diaphragms, cervical caps, and spermicides. They are widely accessible, often available over-the-counter, and offer varying degrees of effectiveness.
Male condoms are the most commonly used barrier method, with a typical use failure rate of around 13%. Female condoms, while less common, offer women more control. Diaphragms and cervical caps require a prescription and proper fitting by a healthcare provider. Spermicides, used alone, are less effective, but can be used in conjunction with other barrier methods to increase protection.
A key benefit of condoms – both male and female – is their ability to protect against sexually transmitted infections (STIs). This is a critical advantage that no other contraceptive method offers. I want to be clear: condoms are the only method that protects against STIs. Don’t skip that.
Proper usage is essential for maximizing the effectiveness of barrier methods. Condoms must be used correctly and consistently, and diaphragms/cervical caps must be inserted properly before intercourse.
Permanent sterilization
For individuals absolutely certain they do not want to have children, sterilization offers a permanent solution. This includes vasectomy for men and tubal ligation (or salpingectomy) for women. These procedures are highly effective, with failure rates of less than 1%.
Vasectomy involves surgically blocking the vas deferens, preventing sperm from being released in semen. Tubal ligation involves blocking or removing the fallopian tubes, preventing eggs from reaching the uterus. Salpingectomy, the removal of the fallopian tubes, is increasingly preferred as it also reduces the risk of ovarian cancer.
This is a big step, and it’s not something to take lightly. Thorough counseling is essential to ensure the decision is fully informed and considered. Recovery times are generally short, but discomfort and swelling are common. Reversal rates vary, and success isn’t guaranteed. A reversal is a complex surgery and doesn’t always restore fertility.
It’s crucial to understand that while sterilization is highly effective, it's not always 100% reversible. Individuals should be confident in their decision before proceeding.
Emergency contraception
Emergency contraception (EC) provides a backup option when contraception fails or is not used. There are two main types: copper IUD insertion and EC pills. The copper IUD, when inserted within five days of unprotected sex, is the most effective form of EC.
EC pills come in two varieties: levonorgestrel pills (like Plan B One-Step) and ulipristal acetate pills (like Ella). Levonorgestrel pills are available over-the-counter and are most effective when taken within 72 hours, while ulipristal acetate pills require a prescription and are effective for up to five days. They work by delaying or preventing ovulation.
Emergency contraception is not an abortion pill. It stops a pregnancy from starting; it doesn't end one that already exists. It is a backup, not a primary method.
This isn't about 'punishment’—it's about having options when things don't go as planned. EC provides peace of mind and control in unexpected situations.
Comparing your options
Choosing the right contraception method is a highly individual process. There is no single 'best' option, but rather a method that best aligns with your priorities and lifestyle. Consider the following factors when making your decision: effectiveness, cost, convenience, potential side effects, STI protection, and reversibility.
The following table provides a comparative overview of the methods discussed. It's important to remember that this is a general guide, and individual experiences may vary. This isn't about ranking 'best' to 'worst', but about highlighting the trade-offs of each method to help you make an informed decision. I want to emphasize that the 'best' method is the one that works best for you.
- Method | Effectiveness (Typical Use) | Cost | Convenience | Side Effects | STI Protection | Reversibility
- IUD (Hormonal) | 0.2% | $300-$1000 (initial) | High | Irregular bleeding, mood changes | No | Yes
- IUD (Copper) | 0.8% | $300-$1000 (initial) | High | Heavier periods, cramping | No | Yes
- Implant | <0.05% | $300-$1000 (initial) | High | Irregular bleeding, mood changes | No | Yes
- Pill | 91% | $20-$50/month | Moderate | Varies greatly | No | Yes
- Patch | 91% | $20-$50/month | Moderate | Varies greatly | No | Yes
- Ring | 91% | $20-$50/month | Moderate | Varies greatly | No | Yes
- Depo-Provera | 94% | $75-$150/injection | Moderate | Irregular bleeding, weight gain | No | Yes
- Male Condom | 13% | $2-$20/month | Moderate | None | Yes | Yes
- Female Condom | 28% | $2-$20/month | Moderate | None | Yes | Yes
- Vasectomy | <1% | $500-$1500 | High | Mild discomfort | No | Generally permanent
- Tubal Ligation/Salpingectomy | <1% | $2000-$6000 | High | Generally low | No | Generally permanent
Contraception Methods for Long-Term Childfree Living: A Comparative Review (2026)
| Method | Effectiveness | Convenience & Reversibility | Hormonal Impact | Additional Considerations |
|---|---|---|---|---|
| Combined Oral Contraceptives (The Pill) | High | Daily regimen; easily reversible | Requires consistent hormonal intake | Requires prescription; effectiveness relies on consistent use. |
| Progestin-Only Pill (Mini-Pill) | Moderate to High | Daily regimen; easily reversible | Progestin-only hormonal intake | Requires strict timing; may be less effective for some. |
| Intrauterine Device (IUD) - Hormonal | Very High | Long-acting (3-7 years); highly reversible | Releases progestin | Initial insertion requires a healthcare provider; potential for irregular bleeding initially. |
| Intrauterine Device (IUD) - Copper | Very High | Long-acting (up to 10 years); hormone-free and immediately reversible | Non-hormonal | Initial insertion requires a healthcare provider; may cause heavier periods. |
| Contraceptive Implant | Very High | Long-acting (3 years); reversible with removal by a healthcare provider | Releases progestin | Requires a minor surgical procedure for insertion and removal; potential for irregular bleeding. |
| Contraceptive Injection (Depo-Provera) | High | Requires injections every 3 months; reversible after cessation | Progestin-only hormonal intake | Effectiveness declines with delayed injections; potential for weight gain and bone density changes. |
| Male Condoms | Moderate | Readily available; no prescription needed | Non-hormonal | Requires consistent and correct use; offers STI protection. |
| Female Condoms | Moderate | Readily available; no prescription needed | Non-hormonal | Requires correct insertion; offers some STI protection, but generally less effective than male condoms. |
Qualitative comparison based on the article research brief. Confirm current product details in the official docs before making implementation choices.
Essential Comforts and Support for Your Childfree Journey

Water-based formula · Paraben-free · 8oz bottle
Enhances comfort during sexual activity, which can be a factor in choosing long-term contraception methods.

Digital menstrual cycle tracking · Personalized insights · Available as a gift card
Provides essential data for understanding reproductive health and timing, crucial for effective contraception management.

XL size for broad coverage · 6 heat settings · Auto-off safety feature
Offers targeted relief for menstrual cramps and general discomfort, contributing to overall well-being.

High-waisted design · Full coverage briefs · 4-pack
Provides a comfortable and secure foundation for daily wear, supporting overall comfort.

Heavy absorbency period underwear · Cotton material · Leak protection
Offers a reliable and comfortable alternative for managing periods, ensuring dryness and confidence.
As an Amazon Associate I earn from qualifying purchases. Prices may vary.



No comments yet. Be the first to share your thoughts!